Science is miraculous….HBOT therapy that reversed brain damage in toddler.
https://m.facebook.com/story.php?story_fbid=1933056560320331&id=1850833625209292
Science is miraculous….HBOT therapy that reversed brain damage in toddler.
https://m.facebook.com/story.php?story_fbid=1933056560320331&id=1850833625209292

Check out our updated Story Submission Page.
Now with Caregiver and Survivor Writing Prompts
You do not have to be a writer to tell your story. Just willing to share it with someone.
Hello there. Thank you for your interest and considering our site www.hopetbi.com to share your story. I would be honored to tell your story as you wish to share it. We are glad to correct spelling so don’t worry about that.
I want you to be able to tell your story your way. Some things to include in your story that people often have questions about, are listed in the questions below….
Please feel free to add more than the questions listed. This is just a helpful starting point for a Caregiver story:
What happened to cause you to become a Caregiver for Polytrauma or TBI?
What injuries did they sustain?
When did this occur (Date or Season and Year, or)
How old were you when you became a Caregiver?
How old is the person who acquired the TBI or Trauma? How many concussions or TBI’s have they had? How old are they now?
How Long was their recovery? If still recovering what are you involved in helping them with, regarding care?
Can you identify what your biggest struggles are or have been over the weeks/months/years as a Caregiver?
What things do you do for self-care (to cope, take breaks, stay refreshed)?
Were you financially prepared to take on being a Caregiver?
Did you have any special training for the injuries of the person you are/were a Caregiver for?
How has being a Caregiver affected your physical and mental health?
Have you had the social support and resources you needed to provide the care needed?
How has being a Caregiver impacted your relationship with that person since their injuries?
Where do you go to connect to other Caregivers like yourself?
What are some of your hope and fears regarding this whole journey as a Caregiver?
Where do you live now (State, Country)?
What do you want other people to know about your experiences?
Why did you choose to tell your story?
What name do you want represented online (first and last please)
Do you have any pictures you want to submit of the before, during, or after? (accident, hospital stay, incident, etc?)
Ways to submit your story:
Who can submit a story? Survivor, Healthcare Provider, Caregiver, Family relative, friend, etc.
Can a story be submitted for someone who has died? Yes, if their story involved sustaining a Traumatic Brain Injury or bodily trauma, and their death was a result of bodily trauma and or Traumatic Brain Injury/Acquired Brain Injury. Please message if you have any questions. You can be the voice of their story if you knew them personally.
Also for you to know…I am not representing any business and there is no compensation for sharing your story. I am a Survivor and saw a need I wanted to help with as much as possible. We post stories on our site to give people a voice to tell their story and a place where others can read it.
E-publish simply means (for our purposes) to post on our site.
As Science evolves, so should the diagnosis and treatment of Traumatic Brain Injuries.

Check out our newly added Web Page: SPECT CT
This is an important second test in settings where CT or MRI are negative after a closed head injury with post-injury neurological or psychiatric symptoms.
So something amazing happened during the last four years, in my recovery process, and through countless hours of rehabilitation. I discovered that with all my new normals, some things remain the same, some things about me are vastly different, and some things have become hugely magnified or what was once dormant is now renewed in a different way. What I am referencing in this particular post is my absolute love and passionate interest in medicine, science, and all that entails.
I find I am at peace the most when learning new material in these topics. This has been my “go to” coping mechanism since I was like 5 years old. Medicine has always been my first love. I have gone away from it, come back to it, gone away from it again. Then when I was wondering just what I should be doing with my life and evaluating whether to have more children, where to take my career, enjoying my job
Some people cope and find their center of “grounding” by running, drinking alcohol, exercising, listening to music, playing video games, communing with nature, watching TV/movies, smoking, having sex, going to church, participating in artistic expression, etc. Me? I find that Medicine, specifically investigative Medicine or investigating medical issues is one of the things that brings me a sense or peace, a sense of purpose, a sense of clarity, a calm.
That being said, in this upside down world of taking back my life from this trauma and all the subsequent experiences since the wreck I was involved in….I find that researching my injuries, how to better my life, how to prove the science behind all the subjective, objective, developmental, and evolving facets of my recovery is how I cope. It has served me well and helped me find the best care, catch the mistakes made by providers, celebrate the things done correctly by providers, find the best providers, realize that even amongst specialists, even the basics can be missed; it has validated many things for me. It continues to enlighten me about the realities of living a new life, and how best to go about it.
Proper diagnosis, proper treatment, and proper documentation cannot be ignored as being imperative and important when somebody endures any medical event or has persistent symptomology. Science is changing and evolving every day. How small, tunnel visioned, limited, and narrow minded we would be as patients, as providers, as attorneys, as caregivers, as case managers, as advocates to ignore the advances in Medicine (both traditional and alternative) and not allow ourselves the freedom to continue to learn, to do no harm, to keep up with current trends, and to evolve into something greater, broader, and grow beyond our proverbial box of comfort?
This website is a part of my legacy. My venture into baring myself openly to all of you who come across this page, who see these words, who read about these struggles, these triumphs. My attempt to help you find resources easier, should you need them. At the very least, maybe understand how multi-faceted and life changing a Polytrauma and/or Traumatic Brain Injury can be.
That being said, if you come across a new article, a new treatment, a new study, a new idea, a new topic you want to see in these pages, a revolutionary sytematic way of addressing recovery and rehabilitation, I would be honored to hear from you and thankful for you sharing what you have found……. with me.
If you have gotten this far down in this post….thanks for sticking it out and reading it. Please share with others. Feel free to leave comments below. I actually read them!
Never give up HOPE!

Hello Folks. I’m back on my blog. YAY!!! While I visit often, I have lots to share with you all, and have much medical information, numerous discoveries, and lots of additions to add to this site over the next several weeks. Now however, I am in a position to express my own personal views candidly and without fear of reprisal about something I have been wanting to for quite some time.
It has been a while since I have posted in my blog here. I wanted to explain that in addition to focusing on my rehabilitation goals, I was also embroiled in a fight for my life with the insurance company representing me in my Michigan NO FAULT claim.

I had sued them for numerous items of service they were not paying on time/stopped paying under the laws that are supposed to, in theory, mandate and compel them to act in a judicious and timely fashion by the letter of those laws.
I, like so many other NO FAULT recipients, suffered additional and repeated traumas at the hands and manipulation of the Insurance Company(ies) that are supposed to be handling the various aspects of our NO FAULT claims. Instead, bills that they are supposed to pay in full, within 30 days of the bill being submitted to them (according to law); attendant care established through a prescription of a licensed physician ( for home health care, nursing care etc) provided by an agency or family member; medical mileage/travel supposed to be reimbursed after it has been incurred; replacement services (household services), wage loss, and other benefits afforded by Michigan law – they ignore &/or pay at their whim…not based on the actual laws. These laws are great on paper, for the constituents, yet there is no accountability for the Insurance companies to be mandated to actually follow the law on paper.
Did you know that the law States that the insurance companies can be charged “Interest” on any bill that is not paid within the 30 day time frame that it is submitted to the insurance company.

Again, this sounds good on paper, right? WRONG! Apparently the manipulation of that law is wholly accepted throughout the whole NO FAULT process as there are currently not any laws in place detailing when or how those interest payments must be paid AND making them non-negotiable items, or compelling them to actually be something the insurance company(ies) wish to avoid, because they would be required to pay that interest. It does not eliminate them from being negotiated away. They can only be charged this “interest” if you acquire an attorney, sue them, AND actually go through a trial where they can still negotiate out of that responsibility. The majority of cases go through a settlement procedure (like mine) and apparently that eliminates all possibility of them every having to pay interest on anything, that by law, they owe the interest on. This abhorrent process is just one of the many things that needs to be reformed in our NO FAULT system. Bottom line….if you don’t pay your bills within 30 days of receipt of that bill, you WILL incur interest for each day that is delayed. That interest should NOT be allowed to be negotiated away in Settlements, Trials, or other modalities regarding the NO FAULT process. This is a willful and purposeful choice they make, knowing there are no consequences. Holding them accountable, will, in theory, allow the NO FAULT system to do what it is supposed to do, take the burden off the individual who was actually in the wreck, so they can focus on their recovery. This would also take the burden off of the Courts being tied up in months or years of the back and forth legal ping pong that these Insurance Companies can afford to play. Reform should be attempting to compel the Insurance Company(ies) to do their jobs …..with our money.
The NO FAULT system through and through is a progressive, positive and integral part of our infrastructure in this State, absolutely worth saving and investing time and money in. It is a system to be envied by all other States and a model worth replicating. However, it is a system that needs transparency across the board, and accountability across the board as well though. After all, fraud and spuriousness is often propagated by the Insurance Company and their agent(s) themselves.
NO FAULT does require reform and clearer lines of accountability for all involved, but specifically the Insurance Providers themselves (obviously I feel this cannot be expressed enough). The very leviathan presence of these companies who with impudent disregard for the Courts, Judges, constituents, and laws voted on and enacted by the constituents (voting citizens) – often find themselves escaping their financial responsibilities, shirking the due diligence required of them, and using subterfuge and prevarication, knowing there is nothing to hold them accountable. Nothing at all. In my opinion, this is the grossest form of medical negligence, injustice, and sheer despicability.
That all being said, I have come to the end of this particular chapter of this grueling process through a Settlement process that was to say the least….less than desirable. Since  the wreck I have literally fought for each breath, each step, each grip, each movement, each thought; each valuable, talented, progressive, and proficient providers; each benefit afforded to me by law, each opportunity to improve and have a decent quality of life. While not easy, while not always positive…absolutely necessary to survive.
the wreck I have literally fought for each breath, each step, each grip, each movement, each thought; each valuable, talented, progressive, and proficient providers; each benefit afforded to me by law, each opportunity to improve and have a decent quality of life. While not easy, while not always positive…absolutely necessary to survive.
I have endured countless days, weeks, months…and now years of acute/chronic pain, loss of body integrity, loss of social confidence, ongoing medical crises, and a complete change in my life, the way I live and relate to others and even relate to myself.
I have been made aware, through my personal experiences, of the dark side of the medical establishment that includes some incompetent  colluding providers “in white coats and black hats (figuratively speaking)”, inaccurate medical documentation, missed/delayed labs, missed/delayed surgeries, missed injuries, delayed treatment,missed radiology exams, and the desperately fallible humanness of those we should be able to trust implicitly with our lives.
colluding providers “in white coats and black hats (figuratively speaking)”, inaccurate medical documentation, missed/delayed labs, missed/delayed surgeries, missed injuries, delayed treatment,missed radiology exams, and the desperately fallible humanness of those we should be able to trust implicitly with our lives.
Despite all of this though….I have learned to advocate for myself on a different level. I have learned I AM a voice for those who are not able to be one for themselves. I have learned that we as a medical society are only just starting to learn about the miraculous processes that make us who we are.

I have learned who my true friends are or aren’t. I have learned that there is always a reason to HOPE and to never give up. I have learned that FAITH and LOVE really does prevail over darkness and injustice.
I have learned that every bit of essence that this blessing of a life has given me by the miraculous opportunity I have been given to survive is something to be protected and coveted. I have learned that sometimes being an honest, honorable, and sincere individual is sometimes just not enough. I have learned that discrimination comes in forms we don’t even talk about as a society. I have learned that I can endure more pain than I would have ever thought possible. I have learned that my life matters and I can find value in the person I am now. I am still learning how I can make a difference in this world and be a catalyst for positive changes and not compromise the core of who I am.
Finding the path to recovery is not just a journey….it is a pilgrimage. I will survive, despite continually traversing all of this Legal Monstrosity.


Believe your body. Trust your body. If something feels “off” then check it out. Be bold. Be brave. Keep striving to find answers to help you live YOUR best life.
Forget the naysayers, those who do not support your personal growth, and those who seek to bring you down.
You do not need to live the life others think you should be living; not the life others want you to live; not the life that cannot be reclaimed in the way you lived it before; not that familiar life from the past that you grieve being lost
This is YOUR life….your NEW NORMAL. Own it. Embrace it. Learn from it. Thrive in it!!!
Your destiny is in your hands. Stay strong. Keep going. Never give up. Be bold. Be different!
#hope_tbi #survivorjourney
#polytrauma
I spent the whole week anticipating when January 4, 2018 would arrive.
I was awake past midnight drinking in the fact it was finally here. I eventually went to bed confident I would wake up again in a few hours. I did wonder if I would feel differently.
It has been 4 years since the wreck happened as of Thursday January 4th, 2018. It has been hard to separate my life from that one catastrophic event and the events that took place around that time. It’s like my body’s cells hold the memories my mind cannot seem to bring to fruition in their entirety….even now.
All day my body ached, spasmed, and refused to cooperate with me. All day, with each deep breath and slow measured movement I was reminded that even though it was four years ago and a different time entirely – the pain goes on.
All day with each deep breath I was grateful. To be able just to breathe and be aware of what was around me seems like such a precious gift. To be able to hear the kids waking me up and to hug them and touch their beautiful faces was such a simple pleasure I lost for a while back then. To walk (albeit slow, painfully, and guarded) around and touch a door, a counter, the wall, a picture, and descend the 13 stairs that always feel like an accomplishment to tackle…going up or down – was a gift I remain grateful for still.
I have a life. No, it’s not my old life. It’s not a life without daily physical pain. It’s not a life without struggles on many unseen levels. Hell, it’s not even the life I wanted, dreamed of, or imagined for myself at this age. It is starkly different. However, it is still valuable. In many ways, even with all the seeming uncertainty my life still matters and I love my life even more.
The value of having love from a person who truly believes you and believes IN YOU cannot be overstated. That love pulled me through dark pain, dark thoughts, and from the other side where HOPE dies, Faith falters, and the darkness of depression laps up the drips of ongoing pain and overwhelming fatigue. Love, patience, acceptance, tolerance, validation, and empathy. I am blessed with these every day from my husband, my mom, my kids, my brother, and most of my providers.
I am stuck. Stuck between true determination, progress, and fortitude and a stagnant knowing acceptance of this pain going on for eternity. Stuck from moving forward as each step forward drags me backwards towards the abyss a little more each time. Stuck being a hypocrite of sorts because I work to find value in the pain and limitations of these disabilities. Even though I find myself begging for relief from my Creator as some days it is too much to bear. Stuck with wanting to work and bring awareness to Polytrauma and Traumatic Brain Injury ….all while having the consistent lack of cooperation from my body, mind, and utter lack of motivation.
I feel relieved for meeting people, groups, and providers who truly value life as I now know it and help me stay on track.
I feel like I should be saying something wise, positive, and upifting today to all of you reading this. Yet I have nothing else but that which I already continue to give. My transparent self.
So much swimming in my head today. So much healing validation. So much continued angst and so much continued life force to pay forward.
Let us remember the 4th Anniversary of my survival, my youngest son’s survival (and that of Greta the other driver). Let us remember that this was the day Caren died four years ago and was brought back; to show that HOPE lives and all things are possible as long as we dont get tunnel vision. With a little Faith and a whole lot of self-determination I embrace the desire to SURVIVE!!!
To all you other warriors out there standing up to your own dark sides and embracing the changes that continue to engulf you…or to those who are helping them face their daily battles….thank you. May you know peace, may you know relief, may my strength be the light saber that helps you find your own independent path as well.
At the end of the day, do your best. Make every effort count and never ever give up HOPE. May the 4th be with you!!!
I just wanted to thank those of you who have signed up on our email notification list here on our website http://www.hopetbi.com
I also want to thank you if you “liked” our page on Facebook and follow the Blog posts. It means a lot to me and hopefully what I write is helpful to you or someone you know in some small way. If you haven’t liked our page on Facebook yet….now’s your chance.
HOPE TBI – FACEBOOK (FB) (online support and information Group)
HOPE TBI Co-Op and Exchange (donate items needed to others, acquire needed items – no selling or vendors allowed here)
HOPE TBI – Facebook Page (we have a Facebook page; this is separate from the Support Group. Remember to “LIKE” us on Facebook)
Follow us on Twitter: HOPE TBI (@hope_tbi)
Contact us: hopetbi4ever@gmail.com
Remember to leave comments after you read an article, whether positive or negative. Your opinions are valuable and I welcome the feedback.
Help me bring awareness to Polytrauma and Traumatic Brain Injury….SHARE SHARE SHARE ![]() 😊
😊
Love you guys muchly. Never give up HOPE!!!

Events are typically considered traumatic when they threaten the life or bodily integrity of the individual who experiences them. After experiencing a trauma people tend to develop certain predictable reactions. Examples are the following:
[while I have no memory of the wreck I was in, since I started dreaming again, I dream of being in wrecks, of my kids or family members dying in wrecks, and am consumed with many unwanted thoughts and various levels of anxiety when in a vehicle that varies from day to day. On my worst days this creates a lot of fear and anxiety]
[I can attest to all of this. This is one of the largest part of my recovery that I continue to work on and that gives me the most challenging hurdles to overcome and deal with]
[ I can’t say that all of this necessarily applies to me. I do like to avoid driving in bad weather, as it makes me quite nervous and fearful. Stop and go traffic heightens my traffic anxiousness, and I have a lot of other challenges while riding as a passenger now…especially]
So, that being said, the wreck I was in was absolutely a traumatic experience.
I always felt I had a high pain tolerance before the wreck. I may have, I did give birth twice after all. Yet now I believe I was mistaken. Childbirth Labor does not compare to multiple fractures and the chronic pain that never goes away from multi-system traumas. At least with childbirth, eventually the pain stops and repeating that process is a choice.
My tolerance for pain has grown ten-fold. What I would have gone to the hospital for before, I wouldn’t even blink at for a Tylenol now. That being said, I have sunk into a new acceptance of this chronic pain filled body I live in now. I accept it as my new normal. My new cloak of pain I have become accustomed to. Chronic pain that some days holds me hostage from accomplishing what I desire. That is, until it raises its ugly head to show me it can still get worse with white hot nerve pain, muscle spasms, and a debilitating wave of continual sharp anchors that drag me down.
I have always had an intuitive relationship with my body. A polytrauma screws all that intuitiveness up. Some days it’s hard to know what is up or down or sideways with where that chronic pain is located. Some days I can point right to its origin. Other times it feels like it is all over me and I can barely walk or pick up my feet.
I have been hurting a lot since I got off of the pain pills on my own. My back aches, my feet intermittently get pins and needles. My right knee doesn’t want to cooperate with that left foot that tends to drag by the end of the day. My neck feels puffy, tight, and just hurts and acts like it has a little storm in there shooting electric lightening bolts down my arm to my fingers and up to my ear now and again. My ribs that are plated, like to play musical ribs for the spasms and often include the right lung and back in their spasm just for fun. My head throbs and I feel such intense exhaustion. Most days, it is a struggle to just get moving. Add that on top of the random high pitched dog whistle sound in my ear/head at inconsistent times. Makes things quite interesting.
I am driving more now too…so that means no muscle relaxers or pain medication while on the road or doing errands. I am strictly diligent about this. Of course, the trade-off to taking on more responsibility is being more irritable, hurting more, having more intense muscle spasms, shooting nerve pain, and dragging myself around literally days and weeks at a time without being able to get on top of the pain and discomfort.

I am a whining mess as I type this as I so get tired of hurting and aching. Here is the irony though. I love being alive so much, and value life so much, that the value of living is worth more than the miserable pain that continues to come in waves.
I got news for ya’ ….Chronic pain threatens body integrity as well. Any new flares that are not the new normal are seriously emotionally and physically exacerbating. It’s like “seriously how much must I take”. So the trauma continues and I remain….Hurtin’ for certain.


As time progressed, as my healing progressed, as I was forced out of the room due to sheer necessity to survive my pain, to attend numerous therapies and medical appointments, and to be a parent – I began to adjust to new tolerances. I also learned rather quickly most of what triggers to avoid so I didn’t end up in a full blown panic and puking my guts up from the dizziness, headaches, and a bouncy massively overstimulating environment.
Getting out of the house is a solid accomplishment. There is a lot of planning that goes into getting out and about. There are things to consider that I took for granted before the Polytrauma. Checklists are my friend. If I deviate from this process we have established, things do not go well at all.
Some days I do better than others. I find I am able to be out longer and more often than even a year ago. However, I recognize that I do not have the same comfort level I used to before the polytrauma and I value getting back home as soon as possible. Some days I still have to force myself to leave my room or go downstairs to the main living area of our home. Some days I feel ready to face the world, get outside, something happens that I didn’t expect and NOPE…back home I go.
Trips away from home, the longer the day, the busier the activity, the longer the recovery time afterwards. A one day trip could take several days to recover from. A day of appointments could take a week to level out from again. If you have back to back appointments or requirements, it becomes a vicious cycle of feeling overwhelmed, incompetent, and beyond exhausted – just weary and pummeled.
So planning in advance, if possible, become a requirement. Having someone help you organize your schedule, your time frames, your goals is imperative to attaining those small victories.
Having things to help you cope in moments you can’t be home is imperative.
 In the beginning I was at the point when I couldn’t easily reset myself, so I would say “BRAIN TIME”, go in my room (or they would have to leave my room), and I would stay there until things settled down in my head. No interruptions, no calls, no questions, door shut. Sometimes this was moments, sometimes minutes, often hours, or occasionally days. I needed absolute silence, a dark room, a warm heavy blanket and to lay down perfectly still. I slept a TON.
In the beginning I was at the point when I couldn’t easily reset myself, so I would say “BRAIN TIME”, go in my room (or they would have to leave my room), and I would stay there until things settled down in my head. No interruptions, no calls, no questions, door shut. Sometimes this was moments, sometimes minutes, often hours, or occasionally days. I needed absolute silence, a dark room, a warm heavy blanket and to lay down perfectly still. I slept a TON.
As time has passed and I am now three and a half years out from my trauma, I still call BRAIN TIME now and again, yet it is less often that it used to be and I have employed other coping mechanisms to help me reset myself.
However, once my brain has decided it has had enough for that moment, or that day. It’s like it’s done “now” and not even I can control the shut down process. I am learning to pace myself still and manage this more effectively. This does not make for a great social life though, I will say that.
After the polytrauma, it was like someone took that inner compass and smashed it. When I tried to lift my head, the room would spin like just got off a tilt-a-whirl on the Gravitron from a carnival. When they would sit me (and eventually after I sat up on my own) I would be so enormously dizzy that sometimes that labyrinth of puking was unavoidable. No to mention the throbbing headaches that seemed to be everywhere and made my forehead feel like it was 50lbs all by itself pulling me forward. The back of my neck ached and I would often have a “belly ache in my neck” if that makes any sense. Looking up and left exacerbated EVERYTHING and so I learned to avoid looking that way.
 Two and a half years after the trauma I started to return to driving. I would learn my inner compass was missing/broken. I was horrified to find myself LOST after taking my kids to school. In fact, I couldn’t remember how to get there….a trip I had made hundreds of times before. I used a GPS because it was like I had never been there before. Now THAT made me feel coo-koo….I didn’t understand. Then I got lost heading home. I literally ended up 20 minutes in the opposite direction because I couldn’t remember what to do or how to get where I needed. GPS became an absolute crutch. As time has gone on, I have gotten better about figuring out my routes. Often times I could think of where I needed to go…yet applying it to real life outside my head was a different reality entirely.
Two and a half years after the trauma I started to return to driving. I would learn my inner compass was missing/broken. I was horrified to find myself LOST after taking my kids to school. In fact, I couldn’t remember how to get there….a trip I had made hundreds of times before. I used a GPS because it was like I had never been there before. Now THAT made me feel coo-koo….I didn’t understand. Then I got lost heading home. I literally ended up 20 minutes in the opposite direction because I couldn’t remember what to do or how to get where I needed. GPS became an absolute crutch. As time has gone on, I have gotten better about figuring out my routes. Often times I could think of where I needed to go…yet applying it to real life outside my head was a different reality entirely.
It is a horrific and scary feeling to feel LOST. I called my husband in tears a few times telling him I didn’t know where I was or how to get home (when phone died and I didn’t have access to GPS). Most times he would answer the phone, sometimes he didn’t hear it and I would be out there in a full blown panic. I would feel scared and the noise around me seemed to get magnified to a level that felt like it was trying to kill me. I could feel myself slipping into this dark space of isolation and I literally couldn’t think of how to fix it. I do not remember how I made it home in those elevated panic times. What I do remember is deciding I couldn’t drive yet and that I didn’t feel safe outside of my house, let alone my room. It has been a massive process to get back to driving again.
Now I am driving more often and the short local routes I do really well at. If I forget I just turn on the GPS. We purchased a charger for the vehicle so I never have to worry about my phone dying (unless the bill doesn’t get paid – GPS doesn’t work then by the way). So the phone is as important as the mortgage for me as far as financial priorities.
Buildings I have been to a lot I still get turned around in since my Trauma. Oddly enough sometimes I get lost in my own neighborhood or kids’ schools. If I survive an outing without getting lost, having a panic attack, or struggling to survive the experience – I consider that a WIN!
 If they turned their backs to me I would ask them to turn around and repeat what they said. Some folks are super accommodating, some act put out by this. Often times folks think you aren’t interested in listening or you do not care about what they said. It wasn’t that, I just couldn’t process what they were saying. Sometimes the words didn’t make sense. It’s like I was listening to a foreign language sometimes. Sometimes it was like I could see their mouth moving, hear noise coming out, yet couldn’t make out the words. This was maddening. Oh! if I was doing something and all my focus was on it (like typing or reading), forget about me hearing you..it just didn’t happen.
If they turned their backs to me I would ask them to turn around and repeat what they said. Some folks are super accommodating, some act put out by this. Often times folks think you aren’t interested in listening or you do not care about what they said. It wasn’t that, I just couldn’t process what they were saying. Sometimes the words didn’t make sense. It’s like I was listening to a foreign language sometimes. Sometimes it was like I could see their mouth moving, hear noise coming out, yet couldn’t make out the words. This was maddening. Oh! if I was doing something and all my focus was on it (like typing or reading), forget about me hearing you..it just didn’t happen.This has gotten better for me in a lot of ways through my rehabilitation journey, not better in other ways – however, I keep learning ways to cope with it despite its abounding annoyance. I am a lot better about being vocal about it though with who I am speaking to now. Once you get used to functioning at a certain level it just becomes your new normal and you accept it as what is.
However after the trauma, that seemed to also have changed. I couldn’t remember how to spell basic words. I find myself misspelling things often and missing the same specific letters when I type. I would look at say……a couch. I could see the word in my head, I knew what it was, yet all I could get to come out my mouth was “that thing there that we sit on”. I have become accustomed to calling things differently than what I am thinking now or what they actually are. Sometimes I come up with some pretty creative descriptions.
 After the polytrauma I seemed to lose the ability to feel hunger or fullness. For some bizarre and I am sure possibly scientific reason I lost my appetite or desire for food in general. No more interests, no more favorites, no more “cravings”, and no more enjoying the things I used to enjoy before. My sense of taste and smell had changed. Some of the things I enjoyed before now repulsed me. Smelling certain types of food cooking was enough to turn me “green” (sick). Just looking at certain types of food was repulsive. The connection with food emotionally seemed to go on vacation. In fact, if I wasn’t brought my meals in those early months and sometimes still…I just wouldn’t eat because I would just forget to eat or have no interest in it.
After the polytrauma I seemed to lose the ability to feel hunger or fullness. For some bizarre and I am sure possibly scientific reason I lost my appetite or desire for food in general. No more interests, no more favorites, no more “cravings”, and no more enjoying the things I used to enjoy before. My sense of taste and smell had changed. Some of the things I enjoyed before now repulsed me. Smelling certain types of food cooking was enough to turn me “green” (sick). Just looking at certain types of food was repulsive. The connection with food emotionally seemed to go on vacation. In fact, if I wasn’t brought my meals in those early months and sometimes still…I just wouldn’t eat because I would just forget to eat or have no interest in it.
As time has progressed, every once in a while I go from no appetite to suddenly HANGRY (angry rage filled hunger – almost a desperate hunger); HANGRY is rare though. More often than not, I forget to eat or have no interest in eating.
I do like some textures or flavors of some things that I never liked before. My family and I equally find this as quite bizarre.
 I have come to realize that my thyroid-pituitary-hypothalmus axis was way off. My hormones were all over the place and apparently I rattled that temperature control center of my brain pretty good.
I have come to realize that my thyroid-pituitary-hypothalmus axis was way off. My hormones were all over the place and apparently I rattled that temperature control center of my brain pretty good.
I still have some great hurdles to overcome when controlling my comfort regarding temperature. At least now I can feel warmth eventually and not be as cold. Sometimes, I even get hot flashes occasionally and naked isn’t naked enough to cool down. More often than not though, I still get cold. Brrrrr’kin is what the kids call it.
So what temperature is it anyway? I am probably not the most reliable person to ask. You might want to check outside…..then let me know.
There are many more nuances that go along with recovering from a polytrauma and these “7 exposed mysteries” are not an exhaustive list, not even for my experiences.
However, they are some of the things that are not necessarily visible changes to anyone who isn’t experiencing them directly and I felt they were worth mentioning. If you are experiencing these things, you are not alone. What you are experiencing is real.
Hopefully, understanding that this is now your new normal will help you accept yourself as you evolve towards your plateau in search for treatment and healing.
The answer to that questions is quite simple for me. it is a resounding and emphatic YES!!!
I am so eternally grateful for the No-Fault system. I sustained a Polytrauma which included multiple orthopedic fractures (5 in my spine alone, ribs, wrist, pelvis, scapula/shoulder, soft tissue injuries, nerve damage, and a traumatic brain injury).
Thanks to Auto No Fault I was able to have the necessary MULTIPLE xrays, CT Scans and lifesaving surgeries to help me survive. I had to go out of State to save the use of my arm due to a shattered scapula as we have no Trauma surgeons in Michigan who were trained to do that repair. Michigan No Fault made it possible for me not to lose all of the function in my right arm. My whole scapula and shoulder had to be rebuilt.
Medicaid and Medicare would NOT have covered this. We would have been stuck in months of pre-authorizations and appeals and I would have died.
I would have left behind my husband (who is also my provider so I could remain at home and not in a nursing home) 6 children, a mother, a brother, a
nephew, and other family. I would have lost the ability to advocate for others and to function at the level I currently function at.
My story would have ended tragically. My story, while yes, tragic and traumatic continues to be HOPEFUL due to Michigan Auto No Fault.
I WILL need surgeries in the future. It isnt IF….its WHEN. Auto No Fault provides me with the medical security to still be here for my children, and hopefully some day….their children.
Please, I implore all voting members to vote
NO ON HB5013
YES on the Fair and Affordable No Fault Reform Plan
You are literally investing in Michigan’s future and survival by voting to save lives and protect the communities you are pledged and voted in by your constituents to serve.
What do you want your legacy to be as a politician, as a fellow human being leaving their mark on this world???
Someone who saved lives and cuts costs by holding insurance companies accountable, or someone who sentenced thousands of men, women, and children to death and financial ruin?
You can be the implement of positive change. You can be a hero. You can be a HOPE’ster.
NO ON HB5013
YES on the Fair and Affordable No Fault Reform Plan
Thank you.
https://hopetbi.com/2017/05/29/be-a-hopester/
UPDATE: 11/2/2017
HB 5013 did not have enough votes to pass. This is great news for the whole State, but especially for the recipients of No-Fault benefits.
Check out our Updated “How You Can Help” page.
Much like the Simon and Garfunkel song…well, back to that in a minute.

So I have always been proud of my muti-tasking abilities throughout my life. Being able to focus in many directions at once and deal with any level of noise without issues. In fact, when I was much younger I used to go dancing and I loved bopping away and really enjoyed the techno beat of the music. I used to be in marching band years ago, Jazz Band, Choir, Show Choir (kinda like Glee for those who have never heard of it) and let me tell you….you just get used to moving, spinning, dancing, and lots of noise. I have always been a lover of music in almost all forms and preferred to listen to music almost all the time.
I loved going to football games,  sporting events, and Pep Rally’s are an amazing memory. As I grew into an older adult some of my music interests changed, yet I still held on to that love of music (which my parents would have probably argued on some days was noise to them). When I worked in Emergency Medicine, I love the sound of the sirens, the pager going off, the squelch on the CB or radios, the multiple directions and decisions that had to be made to save a life. I knew by their sounds whether it was “go time” or not.
sporting events, and Pep Rally’s are an amazing memory. As I grew into an older adult some of my music interests changed, yet I still held on to that love of music (which my parents would have probably argued on some days was noise to them). When I worked in Emergency Medicine, I love the sound of the sirens, the pager going off, the squelch on the CB or radios, the multiple directions and decisions that had to be made to save a life. I knew by their sounds whether it was “go time” or not.
When I met my husband I loved that he played the guitar. My dad used to play all the time and we were a musical family growing up and I was quite ecstatic that I didn’t lose that with marriage. When I became a mother I loved the sounds of my children. All their sounds. From that first cry, to their first words, to their first debate/argument (yes – abhorred and loved at the same time too). I was pretty good about being able to sort and filter out what I wanted to hear and didn’t want to hear merely by choosing…then remembering to finish what it was I was working on (which seemed to be everything all at once). I could talk to more than one kid at a time, answer the phone, stir the dinner I was cooking, with music playing in the background….though admittedly it was often more than one type of music from more than one kid at a time as they listened to their “stuff”. I loved my jobs. I loved working and the business of it all and the multiple directions needed. I was always felt I flourished in tight deadline and crisis situations in the workplace. A lot of times, admittedly – in my younger years, my colleagues found me to be a little “too happy and cheerful”. I heard that a lot. What can I say……I really loved doing whatever it was I was doing at that time.

There was also nothing more spectacular than going to a movie theater with the whole family and listening to the loud blaring beginning of that giant picture on the screen with each thunderous sound from one scene to another. Now that is relaxing!
That is…..until the wreck.
I came out of that wreck different in a lot of ways I still continue to discover. Some things about my personality became enhanced, some disappeared altogether, some new things cropped up that I have been unable to explain. Some things about my tolerance, patience, general mood, ability to withstand hearing things in the same way and do things in the same way changed dramatically. The way I thought about things, processed things, felt things, literally EVERYTHING became like I was experiencing them for the first time……or even worse, not at all. I do not dance anymore. I do not multi-task like I used to, and I do not hear like I used to.
I honestly could not stand noise in any form for a while. Literally, nothing. Just the sound of the nurse’s feet walking in the room and the scuffing of their shoes was overwhelming. The door opening and closing, the beeping and whirring sound of the blood pressure cuff, the constant talking in the hallway, the toilet flushing, people always asking me questions I couldn’t understand or I would answer quickly in the hopes they would soon just be quiet. My memories of the hospital are in and out. I remember voices and feelings more than I remember faces, names, or the day to day stuff that went on. I remember pain. Lots of pain. I was dizzy, head a constant headache, and nope….no music thank you. I also noticed I had a problem with how horribly bright it was everywhere. When they would turn down the lights it was delicious and relieving. Even the red lights from the monitor would hurt my eyes. Those little night lights built into the wall at hospitals….nope, not my friend.
Then I went home. Things were so different. The house looked different as we pulled in the driveway. The sound of the van door shutting, the leaves blowing, the clunk of the wheelchair, the shushing of the adults to the kids as I made my way inside. The days that followed brought lots of appointments and a constant assault on my head, my eyes, and my ears. On top of it all I could “hear” the crunching of my shattered scapula moving with each therapeutic effort. I could hear a high pitch tone that never seemed to go away for the longest time. It almost sounded like a dog whistle or a fine squealing. It was awful. I noticed that while I had this going on, it sounded kind of muffled at the same time and it became difficult for me to focus on words, sounds, and more than one noise, or more than one person talking at a time was enough to send me into tears.
As time passed I noticed it helped if I read  people’s lips to understand what they were saying. Sometimes still I will see lips moving, know they are talking, yet understand NOTHING. I have learned to ask for repetition a lot. Sometimes I just act like I know what they said….nod….and smile. I learned little tricks, like wearing earplugs, sunglasses, carrying a blanket to cover my head with, lots of those types of things to cocoon myself from the auditory assaults of whatever environment I was in. Continue reading
people’s lips to understand what they were saying. Sometimes still I will see lips moving, know they are talking, yet understand NOTHING. I have learned to ask for repetition a lot. Sometimes I just act like I know what they said….nod….and smile. I learned little tricks, like wearing earplugs, sunglasses, carrying a blanket to cover my head with, lots of those types of things to cocoon myself from the auditory assaults of whatever environment I was in. Continue reading

There is a chain of events that happens with an auto accident that involves serious injuries, polytrauma, or death.  A ripple effect that swirls and snatches and seeks to destroy not just the patient, but the family, the spouse, and friendships of that patient as well.
A ripple effect that swirls and snatches and seeks to destroy not just the patient, but the family, the spouse, and friendships of that patient as well.
First, there is the initial accident. This not only causes the injuries, but causes a multitude of mental stressors as well. Fear, anger, shock, disbelief, numbness, sadness, enormous helplessness and grief. If the person survives there are things that help relieve those stressors – such as gratefulness, happiness, apprehension, confusion, hope, and for some, a distinct solidification of their spiritual base.
The stressor for the patient is that the accident itself has happened to begin with; thus causing a multitude of injuries that may affect more than one aspect of their life. They may have memory and cognitive issues in addition to orthopedic injuries. They may have behavior changes and appear to be a different person than they were before the auto accident.
The person may or may not have support and help from a trusted circle of family or friends as they fight to survive, exist, and recuperate. After a while though, often times, friends disappear. Sometimes, the burden is too big to understand or absorb for family as well. A catastrophic injury absolutely shows you the genuineness of the people around you. Life continues to move on without you and you become acutely aware of this. The relatives, coworkers, friends who were supportive at first…eventually go about their lives and forget that you are there….still struggling. The patient is left circling in the same spot, sometimes for months at a time.
Every stressful event that happens AFTER the accident compounds and slows the recovery process and adds to the mental and emotional stressors in the patient and their relationships with others.  Any delayed treatments, or misdiagnoses, or haggling over care of the patient (whether by the family or the patient themselves) causes additional added stressors, which impacts the ability to heal in a timely fashion.
Any delayed treatments, or misdiagnoses, or haggling over care of the patient (whether by the family or the patient themselves) causes additional added stressors, which impacts the ability to heal in a timely fashion.
Something not often talked about or studied is the real impact that Polytrauma and Traumatic Brain Injury has on the spouse or children of the patient. There are changes that happen in those relationships. The household dynamics may change significantly leaving the family feeling disorganized and broken.
Children may feel insecure, may blame themselves, feel helpless and hopeless about their parent’s recovery or their parent’s relationship. They may act out in ways they did not used to. They may regress in their development, they may become isolated or clingy. They may try to act in a parental role with siblings themselves.

They may find ways to cope that are not healthy. Some kids are able to adjust to the changes going on with their parents with lots of support, education, explanation, and patience. Some are not able to adjust. Sometimes the injured parent is too different for them to understand. Sometimes witnessing the changes in their parent is too painful. Sometimes a spouse or child can incur secondary trauma/PTSD as their loved one recovers.
The dynamics in a marriage are also hit with one wave after another depending on the level of injuries a patient has and how severe they are. In a polytrauma or with a traumatic brain injury, often times spouses are forced to take on the previous responsibilities of the patient (household duties, scheduling, transportation, budgeting, cooking, cleaning). This may overwhelm the spouse if they previously depended on their now injured spouse to handle those responsibilities.  The financial stress will compound quickly. The person injured, if a working parent, may be unable to return to work for a period of time…if ever. This creates a massive financial dynamic shift for the whole family. If insurance is not available, or does not cover all of the medical bill this can spell financial ruin for a family. Not many individuals or families are in a financial position to endure a catastrophic injury/event. This is only compounded when the parent that is left working loses their employment because they are taking too much time off work to care for their spouse/family member. This can exponentially compound the stressors in the household.
The financial stress will compound quickly. The person injured, if a working parent, may be unable to return to work for a period of time…if ever. This creates a massive financial dynamic shift for the whole family. If insurance is not available, or does not cover all of the medical bill this can spell financial ruin for a family. Not many individuals or families are in a financial position to endure a catastrophic injury/event. This is only compounded when the parent that is left working loses their employment because they are taking too much time off work to care for their spouse/family member. This can exponentially compound the stressors in the household.
Even the kids can be affected by the financial changes both directly and indirectly. A family may have to go to food banks, acquire assistance from agencies for bills, food, utilities, transportation, etc. Some may end up losing their homes and become homeless. This is a dynamic ripple affect that goes beyond the initial injury at the time of the accident. This ripple affect can continue for weeks, months, or years.
Brain injury often brings on drastic personality changes, which may include irritability, depression, limited awareness of injury-related changes, and argumentativeness.

Some spouses may feel like they are married to a stranger.
They become concerned about whether their spouse will ever be the same again. The reality is, they will not.
The working spouse may feel alone in the marriage or like a single parent (if they have kids) due to the inability of the patient to take on the same responsibilities and roles as before. The non-injured spouse may also lose their marital benefits for an undetermined amount of time. The loss of a partner that they previously shared comfort, affection, mental support, and did activities with. This can put another layer of strain on the marriage, which is now no longer, a normal marriage.
While most people, in an ideal environment without financial devastation and strong support systems in place, progress in their healing over time in a seemingly more timely fashion; a patient with all these added stressors can actually see a delay or lengthening of their recovery period, an exacerbation of some of their symptoms and the real potential for more permanent disabilities. Some patients may even develop mental health challenges in relationship to adjusting to their life of “new normals”. Coming to grips (acceptance) of their injuries, limitations, and the domino affect of seeming losses from their injuries, can be crippling and make the patient and their caregiver feel isolated and in a constant “survival mode” state.
The team in place to help the person recover should absolutely include their providers, and include the insurance company handling their claims as well. Any delays or standoffs regarding reasonable and necessary patient care only seeks to elongate and sabotage the patient’s recovery and future progress.
The ripple affect continues. The waves of pain also continue, yet the tsunami of numerous medical appointments lessen as time goes on. The relationships the patient is left with will continue to shape the shores of their life as they now know it. Some relationships will erode over time, some will get swept away by the current of recurrent trauma’s, some will stand the test of time and hold strong and true.
These moments. The moments that are not measured by the number of breaths we take, but rather the moments that take our breath away are the ones that leave us grateful for being able to wake up to the ripple of a brand new day.


Check out our newly updated webpage about scapula fractures and shoulder injuries from trauma.
SHOULDER INJURIES FROM TRAUMA – SCAPULA NONUNION


“You treat a disease, you win, you lose. You treat a person, I guarantee you, you’ll win, no matter what the outcome.”
~ Hunter Patch Adams
Check out our latest Web Page addition. “Flail Chest and Rib Plating”
https://hopetbi.com/neuroscience-and-polytrauma/polytrauma/flail-chest-and-rib-plating/

#hope_tbi #flailchest #ribplating #polytrauma
Leave us a Comment Below….
Vision and Sensory Center – Cutting edge of current science and treatment of traumatic brain injuries.
https://www.facebook.com/Vision-and-Sensory-Center-1822007318073764/
Chronic Pain Is No Joke!
So it has been 3 years 5 months and 26 days since the wreck I was in. I just call this 3.5 years to round up when talking with people now.
So much has changed in that 3.5 years….and continues to. The time I have spent adjusting to living with that pain will I believe be lifelong. I have come to believe that pain is a lot like grief, just in a different form. Like grief, there are various stages (also much like grief).
Grief Stages Denial, Anger, Bargaining, Depression, Acceptance
Denial & Isolation with Chronic Pain
The first reaction to learning about trauma is to deny the reality of the situation. “This isn’t happening to me, this can’t be happening to me. I don’t have time for this to happen to me,” – though I think I skipped this first stage initially since I was so out of it. I don’t think I had any ability to conceptualize what I had going on with me…..at least not fully. If I didn’t skip it, I don’t remember experiencing this as a first emotion.
I have always known throughout my life that it is a normal reaction to rationalize overwhelming emotions and to push away dealing with them for most people. This allegedly helps carry us through the first wave of pain or shock. However, when dealing with Chronic Pain that is caused by bodily trauma there is not just one wave or an “initial wave” – there is simply….just…..PAIN.
The reason I said that pain is a lot like grief because pain comes in all forms. Orthopedic, muscular, nervous system related, brain/mental system related, endocrine systems, digestive system, reproductive system, literally every part of the body is engaged in this trauma when dealing with a Polytrauma and Traumatic Brain Injury. Each system can be going through it’s own forms of “grief” or “changes” or they can all be happening at once….overwhelmed…..frozen…..stalled….or shutting down in response to the trauma.
Attempting to take all that in and learning that no one around you really truly understands is incredibly isolating. Being unable to put to words how you are feeling when you have never been put into a place in your own life to need words to describe such a horrific continual experience feels isolating. I would deny deny deny that this was actually happening – yet the pain made that reality absolutely undeniable. All I could think of was PAIN….where the hell is all this pain coming from? There was so much I couldn’t pinpoint a starting place. It was like someone wrapped me in a warm pain blanket that was turned up to the highest level possible without relenting for months and months (literally)
Anger with Chronic Pain
As the effects of denial and isolation change in their dynamic, reality and its pain re-emerge stronger than ever. I admit I was not prepared for this emotion which continually hits me in random waves. The anger may be aimed at inanimate objects, our healthcare providers, complete strangers, friends or family. Anger may be directed at the person we perceive that hurt us or even angry at ourselves. Often times feeling guilty accompanies being angry and for some people, this makes them angrier. Sometimes being angry is a side affect of the trauma….especially if dealing with a head injury and the emotional center of the brain has been damaged.
As anger relates to chronic pain though – at least for me, the anger comes from not being able to do what I used to do. Anger at having this affect my life, my mobility, my independence in caring for my own body, and change my normalcy to something I no longer recognized. Anger at literally feeling like a prisoner in my own body and having expectations that are not realistic for the healing required for the injuries themselves, or my ability to deal with the injuries. Anger about missed injuries, or those that are not healing as planned. Angry at feeling dismissed, not taken seriously by anyone outside of ourselves when I say I am hurting. Angry about being financially destitute and unable to provide for my family the way I used to. Angry that I am hurting at all.
Some things that come with chronic pain and anger
Bargaining with Chronic Pain
The normal reaction to feelings of helplessness and vulnerability is often a need to regain control. Let’s face it, with a polytrauma where you cannot walk/have difficulty walking, where you have to have someone feed you, dress you, wipe your butt for you, bathe you and leaves you feeling completely helpless – is a complete loss of control in its most humbling form
Admittedly I have always had a leadership/controlling personality. I enjoy doing a job well and got value from how others viewed my ability to lead, accomplish, and successfully complete something. I loved my independence and enjoyed working and breaking new ground in almost every aspect of my life. Now I am trying to reinvent me.
Then BAM – chronic pain comes in and strips down any ability to control…at least completely what’s going on in your own environment – your own body. This is truly where things spiral a bit…I personally tend to get consumed with dark thoughts and overthinking my care or lack thereof. I think about how I can negotiate better treatments, better documentation, a better more proactive diagnosis. It becomes almost obsessive. I have to admit that there is a fine line between bargaining and advocacy for oneself (which has actually served me well orthopedically). However, along with bargaining comes some pretty repetitive self-talk. This can be a strength and a weakness in the recovery process.
There are many types of depression out there. There are 2 types of depression when dealing with grief and loss that appear most often though. The first one is a reaction to relating to the loss. Sadness and regret predominate this type of depression. We worry that, in our grief, we have spent less time with others that depend on us. This phase may be eased by simple clarification and reassurance. We may need a bit of helpful cooperation and a few kind words.
The second type of depression is subtle and, in a sense, perhaps more private. It is our quiet preparation to separate and to bid our old self as we knew it farewell, while dealing with our “new normal” and the chronic pain that we now live with.
With a polytrauma or traumatic brain injury a person is often on a lot of medications to control various injuries or mood disorders. Some of these medications can actually cause depression. It is hard sometimes to tell where the depression is coming from and requires a thorough awareness of the patient’s medical history. When dealing with depression in myself I learned my depression was there due to many factors – all secondary to the wreck and the ripple affect of all the injuries. I got news for ya’ – peeing yourself in public because you aren’t able to get to the bathroom fast enough when that urge hits ya, living with a chronic headache pattern, chronic pain, and short term memory loss can be very depressing in and of themselves – and that’s just the basic stuff. Now add money problems because you cannot work, being unable to pay bills on time, and all the other normal life stressors which now seem bigger than the pain some days and that depression can drag you down like a cinder block tied on your back while you are in life’s swirling pool.
Seeing your friends lives go on, seeing your family move on while you seem stuck in the same vicious circle – wake up pain, walk – pain, exercise – pain, carving your way through the day until you can go to sleep to hopefully escape pain – (some days that actually works…… over time….until a pain flare)
When depression hits me hard, I notice that grief that holds hands with depression has a bit of a tighter grip. Sometimes this stage feels as though it will last forever and can feel truly overwhelming. I also notice that depression is harder to control when hurting. So being in chronic pain is often not necessarily related to a mental illness (though can be related to endocrine and hormonal imbalances caused by trauma as well), but rather a response to hurting so much for so long and feeling frustration over adjusting to that “new normal”. I also have realized that my pain tolerance has changed dramatically over the last 3.5 years. I can withstand a lot more pain that I used to on some levels – not so much on other levels. I also notice my depression has changed with that adjustment.
Also, by golly, depression is an appropriate emotion when experiencing great loss. A lot of people….professionals even – act like it is some kind of an unnatural process. That cloud of intense sadness that consumes one’s being when they feel like they are all alone in their experiences and realize that their life will forever be dramatically different is a real sense of loss. I really have to guard myself against that whole feeling of “what’s the point in living” “why did I survive” “what am I here to accomplish” and force myself to focus on positive self-talk.
Depression is not a “state to be fixed”, something to “snap out of”. Though I do believe it is important to recognize that our feelings are very real, but do not always tell us the truth about the situation. Grief is part of the healing process. Chronic pain is part of my life now. Some days I manage it better than others – some days….not at all. If grief is a process of healing, then obviously depression is just another important step on that journey. Allowing myself to experience it (yet not get stuck in it) is also an important part of that process.
Depression is also not consistent and can last a few moments to never ending cycle from day to day. It’s okay to cry here and there for 5-15 minutes at a time my counselor told me. That is healthy. It’s a problem though to be really addressed if it consumes your life so much you can do nothing else because of feeling so depressed. If all I can do is think of the depression and cannot quit crying and am withdrawing so much that I am neglecting myself (eating, hygiene, activity participation), then more professional help may be needed.
Not everyone is able to reach this stage. I still struggle with this stage myself on a daily basis in my rehabilitation process. My counselor calls my ability to accept the changes to my life, my body, my new normals as a need to have “radical acceptance”. Let’s face it….something radical has happened to me and therefore requires a radical form of acceptance.
Sometimes seeing beyond our anger or denial makes this more of a difficult process. This phase is marked by being calm. This is not necessarily a period of happiness and it is imperative to distinguish this from the apathy or withdrawal that I spoke about in depression.
So what does it mean anyway to have a radical form of acceptance?
Radical Acceptance to me, means completely and totally accepting something from the depths of my soul and with mind and whole beingness. I have to face the reality that I may never be able to work in the same way that I used to. I have to accept that I am at my medical best in some things, still improving in others, and that yet others may never improve (or may even get worse). It means accepting I may need to use a cane, go to counseling, change the way I do things. It means accepting that chronic pain is just a part of my life now and learning to work around it as best I can. It means knowing that my nerve damage may never heal (or it might) and accepting that. It means to stop fighting reality.
Radical acceptance means that I do not allow myself to feel that rageful anger in my stomach when I am unable to do something I used to be able to do. It means not seething with resentment or bitterness when I see others who have similar injuries doing more than I am capable of with my own body. Radical acceptance means, learning as much as I can, teaching others to do the same, and moving forward with my life.
Radical acceptance is way easier to talk about and understand than it is to actually put into practice in every moment of every day. There are a ton of obstacles that come up to challenge accepting where I am at now. I do know that if I stop fighting all of this, eventually I will suffer less.
What Radical Acceptance is not: It is not giving up. It is not tolerating being mistreated or accepting a misdiagnosis. It is not stopping the ability to advocate for oneself or others. It is not just accepting diagnoses as they are without researching the options thoroughly. It is not giving up on caring about or speaking up for myself or others. It is not about being as silent as a church mouse in a corner with no thoughts and ideas of my own. It is not about even….. being Radical (which some interpret as crazy, out of control, explosive, or some other such adjective).
Summary:
Coping with a polytrauma, traumatic brain injury, any type of grief, and loss really…. is ultimately a deeply personal and singular experience — nobody can know EXACTLY what you are going through.
There are many stages we all go through in our recovery process. These stages closely resemble the stages of grief. There is no set time frame assigned to experiencing each stage, or a particular order in which we experience these stages. Sometimes a person may never get to the Acceptance stage. This is however, the goal for myself.
Acceptance is often misinterpreted by others as the person being “all right” or “okay” with what has happened to them. This is not the case. Some people reach acceptance right away. Most people though don’t ever feel okay for years, if ever. By achieving a level of “acceptance” a person is choosing to learn to live with their new normal self and move forward with their life.
It is not uncommon to repeat the various stages or be focused on one particular stage. Chronic pain can directly affect the way a person processes these stages as well.

What Exactly is “Standard of Care” as it relates to the medical community?
The “medical standard of care” is typically defined as the level and type of care that a reasonably competent and skilled health care professional, with a similar background and in the same medical community, would have provided under the circumstances that led to the alleged malpractice.
A diagnostic and treatment process that a clinician should follow for a certain type of patient, illness, or clinical circumstance.
The level at which the average, prudent provider in a given community would practice. It is how similarly qualified practitioners would have managed the patient’s care under the same or similar circumstances.
**********************************************************************
I have learned over my entire life through various experiences; also being in the medical field for most of my adult life as a healthcare provider in some way, shape, or form that the Standard of Care is as varied as each personality that goes along with the person representing that Standard of Care.
When I had patients I always tried to give them the best of me and my knowledge of my acquired training at that time. When I came across something I didn’t know (which was a continual learning process for sure)…. I immersed myself in learning about the things I didn’t know how to answer for what I was specializing in at that time. That was my way of making sure that I didn’t have that same issue come up again. I guess I just assumed (yes, we know the misnomer of what assume means) that this is how all people sought to learn when they had a passion for medicine. Specialists in a field even moreso…beyond the norm even.
Specialists, surgeons, Department heads I guess I always expected more of those folks. Surely they kept up on all the latest trends, the newest studies, the symptomology associated with the topic(s) they specialized in. Surely they could spot a problem, would assure that the best outcome for the patient was acquired, especially in favor of positive outcomes with their name attached to it.
Surely I could look at them, listen to them use my voice to communicate with them, and trust they knew what they were talking about because after all, their fervor and thirst for knowledge was above and beyond what the average medical professional entailed. Certainly more than what I was trained to know.
So it only made sense that on that fateful day when I became the voiceless patient, clothing cut off to stark nakedness in an emergency room with massive injuries, multiple broken bones, head injury, and clinging to life with each labored breath…..that the sheer mechanism of injury (severe car wreck with ejection and other driver pinned and needing to be cut out) should have demanded a certain Standard of Care from every provider I came into contact with, within that first year, and every day after that.
I have had some really great providers. I still have some great providers. I want to say that first. There are a handful who have done their due diligence and even exceeded the Standard of Care. They are the ones that listened. That actually enjoyed their job and their patients. They are also the ones that keep up on the current and updated things in medicine, ironically enough. They are the ones who think of ways to make things happen instead of making excuses of why they cannot make things happen. They are the providers that never give up on you and take risks to better your quality of life. They are few but mighty. These are the providers I have learned a lot from and have enormous respect for.
The providers who fell short on their Standard of Care, or didn’t even attempt to live up to it….. Those providers left me impacted in ways that created a ripple affect that delayed my care, caused me further injuries, and exacerbated things for my recovery process….and not in a positive way. They are the providers who didn’t listen. Who jumped to conclusions based on opinion rather than facts. They fed off of other reports by other providers that also did not care, did not document properly, or dropped the ball in some fantastic and important way; perhaps even adding wording that invalidated the injuries that actually were quite legitimate and yet ignored. These are the providers that I felt I knew more about my care and the latest treatments available than they did (yes even if they touted themselves as specialists in that field). These are the providers I lost respect for, or never had the chance to establish such for.
The Standard of Care cannot be overstated in its importance. If you specialize in a field, learn all you can about that field. Study it, know it, and be willing to learn more about it. Medicine is changing daily and if a patient brings you the current studies, be grateful. If they discuss them with you and you have never heard about them, go look them up and research them yourself. Knowledge can only make you better at your craft. If you cannot listen…truly listen to your patient when they say they are still suffering – you are in the wrong line of work. Go on a quest, do no harm, and advocate for your patients.
The Standard of Care echoes through many professions, yet in this particular post we just address the medical view as a patient, medical advocate, a Survivor.

A HOPEster is anyone who is interested in helping one person succeed to be independent – even if the person they are currently helping is themselves (specifically related to Polytrauma and Traumatic Brian Injury – though can apply to anything other than these two things as well).
A HOPEster is someone willing to share information, offer support (whether that be emotional, mental, physical, or just by sharing awareness information), and encourages advocacy (self-advocacy, medical advocacy, advocacy awareness).
A HOPEster is someone that thinks outside the box, is passionate, idealistic, and believes in the inherent goodness of others and our collective responsibility to each other as human beings.

(right click on picture to save to your device or share link in above web browser)
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
Reviews and Testimonials
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
Hello There HOPE’sters. We are thrilled to announce 2 awareness ads for this website for you to share in emails, in your social encounters both online and offline.
Below each video is a description of what the video is about and why it was created.
Feel free to click the “SHARE” button in the top of which video you like the best, to choose the sharing option you prefer. SHARE SHARE SHARE….help us bring awareness to others.
This one was created with the thought in mind of how we can overcome anything with the right attitude, with awareness/education, and with proper support. Support can come in the form of friends, family, providers, and even our own children. It is important to remember to find our smile, to love, to laugh, and to embrace life and live it to it’s fullest – in spite of our seeming limitations and new realities. That, in the end, we will be okay – because we have each other – we will overcome!
(of course bubbles always represented to me, a time of innocence, frivolity, and life’s possibilities – you never get too old for bubbles)
This one was created first and the song’s theme is “I will fight for you”.
I created this website with the idea of healing and fighting for myself and my recovery by learning and documenting as much as I could about my injuries…and then documenting what I had learned from my own experiences, documented research, and subjective interpretations. I created the website with the desire of helping to fight for others with similar injuries (polytrauma or traumatic brain injuries) and help bring Awareness to as many people as possible. I want it to be a global reach that says:
“Hey, you are not alone out there in your recovery. You are not alone as a caregiver or a provider – you are not alone with the questions you have, the symptoms you feel, and the life you are struggling to make work for yourself or others”.
I want this video to be something that is remembered. Whether you hear the words “I will fight for you” as a song to yourself in your own mind to help you keep going – because your life is truly worth living; or as a representation of your desire to support and advocate for others….that you will fight for them, no matter what; or as a reminder that this site is a place you can come to share, get information, and feel like you are in a place that cares and understands.
The blooming flowers in the video are Cherry Blossom Trees. This has been symbolic for me for quite some time now. See our page under CHERRY BLOSSOM TREE PICS.
(any ideas or comments welcome – please post them below or email us through our Contact page)
Remember that our Veterans often suffer Polytrauma and Traumatic Brain Injuries in the course of battle in defending our Country and are often put into a position of representing our citizens abroad. They are often put in harms way for the sake of the ideal of standing for the greater good and advocating and doing the proposed right thing.
Let us remember them honorably…those who have gone on before us and given their life in service to others.
The ones that make it home from battle are left to endure the lifelong effects of these life changing events, as are their families with a system that is ill-equipped to handle the atrocities of the perils of war and conflict. We have come so far over the several generations that extend before our existence. Our goals should always be to do better than the generation before ours and learn, strive, advocate, and grow – not just as individuals, but as a Nation.
The Veteran’s that don’t make it home, we, as a Country continue to remember.
HISTORY OF MEMORIAL DAY
Memorial Day is an American holiday, observed on the last Monday of May, honoring the men and women who died while serving in the U.S. military.
Originally known as Decoration Day, it originated in the years following the Civil War and became an official federal holiday in 1971.
The date of Memorial Day (also called Decoration Day), was chosen because it wasn’t the anniversary of any particular battle.
For decades, Memorial Day continued to be observed on May 30….. But in 1968 Congress passed the Uniform Monday Holiday Act, which established Memorial Day as the last Monday in May in order to create a three-day weekend for federal employees; the change went into effect in 1971. The same law also declared Memorial Day a federal holiday.
Many Americans observe Memorial Day by visiting cemeteries or memorials, holding family gatherings and participating in parades. Unofficially, it marks the beginning of the summer season..
For more extensive history on this somber holiday…check out http://www.history.com/topics/holidays/memorial-day-history
To all those who serve, or have served….THANK YOU!
Check out our latest page compiled/completed about Obesity Brain Injury and Trauma
If you have anything you would like to contribute, please let us know.
Let me know if you have any questions about my experiences. I still have a long way to go….however, I am here…alive and able to complete my life journey…now with the use of both of my arms; man does it feel good to be able to hug with both arms again!!!
Never give up HOPE.

Brain Injury does NOT equal Lack of Intelligence
Unless there is objective evidence of brain injury on MRI or CT Scan (hemorrhages, hematoma’s penetrating skull fractures into the brain, etc) people assume the individual expressing symptoms of a traumatic brain injury is faking, exaggerating, or malingering their injuries or the person has psychological problems that had to have pre-existed before their accident. The reality is that the majority of mild (mTBI) and moderate brain injuries show normal results on an MRI and CT scans. They do not show diffuse axonal injuries nor do they show levels of intelligence. Keep in mind also, that women also tend to have longer recovery times than men with regard to brain injuries as shown in recent studies.
Diffuse axonal injuries (DAI) are caused by acceleration, deceleration, and contact forces. DAI affects individual nerve fibers which can lead to a disruption in nerve communication. DAI is microscopic damage to the axons in the brain neural tracts, corpus callosum, and brainstem, is associated with significant mortality and morbidity. When these forces are great enough it creates a shearing force that severs the axons of nerve fibers, which causes nerve cells to die and can create swelling in the brain. The main symptom of diffuse axonal injury is lack of consciousness, which can last up to six hours or more. A person with a mild or moderate diffuse axonal injury who is conscious may also show other signs of brain damage, depending upon which area of the brain is most affected.
Diffuse axonal injury causes cognitive, physical, and behavioral changes that compromise social reintegration, return to productivity, and quality of life of patients and their families. These changes persist beyond the acute phase of treatment and continue for a long period after the traumatic event. Diffuse axonal injury, and more generally TBI, often results in physical, cognitive, and behavioral impairments that can be temporary or permanent.
Due to the diffuse and microscopic nature of the injury, CT scans and general MRIs are typically negative unless small areas of bleeding within the brain are noted within the cerebral cortex or corpus callosum (tracts of white matter in the brain). If a patient presents with unconsciousness and these tests are negative, the medical facility should move onto a different imaging technique to check for DAI. Depending on the severity of the injury and the extent of the damage. A concussion can be considered a mild case of shearing brain injury. At its mildest, DAI can occur unnoticed.
Someone with diffuse axonal injuries that don’t’ show on an MRI or CT scan may also have  brain inflammation or swelling. This can lead to restricted blood supply to the brain tissue and brain herniation. Tonsillar herniation is a type of cerebral herniation characterized by the inferior descent of the cerebellar tonsils below the foramen magnum. Chiari one malformation is a form of tonsillar herniation and is now known to be caused by trauma (like severe whiplash and traumatic brain injury) or in most cases “symptoms awakened” from trauma. This is an often overlooked correlation between trauma and DAI and TBI.
brain inflammation or swelling. This can lead to restricted blood supply to the brain tissue and brain herniation. Tonsillar herniation is a type of cerebral herniation characterized by the inferior descent of the cerebellar tonsils below the foramen magnum. Chiari one malformation is a form of tonsillar herniation and is now known to be caused by trauma (like severe whiplash and traumatic brain injury) or in most cases “symptoms awakened” from trauma. This is an often overlooked correlation between trauma and DAI and TBI.
The occurrence of DAI depends on the mechanism of injury; it is more common in higher energy trauma, especially traffic accidents. Someone who has incurred high velocity trauma, blunt force injuries, or multi-system traumas often have post-traumatic amnesia (PTA).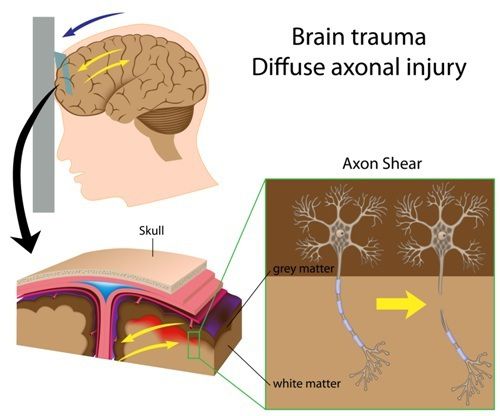 PTA is another good estimate for severity of a brain injury. Anytime a person has a major blow to the head he or she will not remember the injury and related events for some time afterward. People with these injuries might not recall having spoken to someone just a couple of hours ago and may repeat things they have already said. This is the period of posttraumatic amnesia. The longer the duration of amnesia, the more severe the brain damage.
PTA is another good estimate for severity of a brain injury. Anytime a person has a major blow to the head he or she will not remember the injury and related events for some time afterward. People with these injuries might not recall having spoken to someone just a couple of hours ago and may repeat things they have already said. This is the period of posttraumatic amnesia. The longer the duration of amnesia, the more severe the brain damage.
A brain injury does not necessarily affect intelligence. Intelligence is a stable trait which includes many aspects of cognitive functioning. Following a traumatic brain injury, the brain is unable to function as well as it did prior to injury. This is why we typically see some difficulties with memory or academics. However, once the brain recovers there is no change in a person’s overall intelligence. Your intelligence is based, depending on the definition of intelligence, on the son total of your knowledge.
Someone’s IQ can be unaffected by a TBI, but other parts of the brain that “pilot” or guide one’s brainpower can be messed up. Decision-making and complex social interactions can cause major problems in one’s life and career. The individual with high intelligence may still have cognitive problems such as headache, difficulty thinking, memory problems, attention deficits, mood swings and frustration. These injuries are commonly overlooked, especially in those with high intelligence. Their low threshold of functioning or slower processing speeds may appear as average where prior to injury they would have tested as above average..
The brain of the intelligent person is more complex in appearance, not as soft, and has greater weight relative to size. Additionally, it can be noted that the intelligent brain may have an enlarged prefrontal cortex or parietal lobe relative to other areas of the brain. More intelligent people have more wires, more connections and more complex architectures in their brains. These are reflective of genetics, as well as developmental experience.  Also, more intelligent people may enjoy higher processing speed or impulse conduction in brain-wires (axons). But with more complexity in the brain, the net result still could look in performances as much slower decision making resulting in a dulled sense of self, lower test scores compared with their education/experiences, and reduced overall performance compared with their performance before injury.
Also, more intelligent people may enjoy higher processing speed or impulse conduction in brain-wires (axons). But with more complexity in the brain, the net result still could look in performances as much slower decision making resulting in a dulled sense of self, lower test scores compared with their education/experiences, and reduced overall performance compared with their performance before injury.
That being said, Intelligence and personality dysfunctions after minor traumatic brain injury (TBI) (whiplash; slight head impact) incurred in a motor vehicle accident (MVA) were studied in adults after an average interval of 20 months. There was a mean loss of 14 points of Full Scale IQ from estimated preinjury baseline IQ determined from the standardization group (WAIS-R) without evidence for recovery. Personality dysfunctions included cerebral personality disorder, psychiatric diagnosis (30 of 33 patients), post-traumatic stress disorder, persistent altered consciousness, and psychodynamic reactions to impairment. Cognitive loss is caused by interaction of brain injury with distractions such as pain and emotional distress. Unreported head impact and altered consciousness at the time of accident contribute to the underestimation of brain trauma after minor TBI.
Just one concussion can lead to a decrease in brain volume, according to a new study in the journal Radiology.
Specifically, researchers from New York University’s Langone School of Medicine found that people who had suffered a mild traumatic brain injury and experienced symptoms of the injury a year later also experienced brain atrophy (brain shrinkage).
“This study confirms what we have long suspected,” study researcher Dr. Yvonne W. Lui, M.D., assistant professor of radiology and the neuroradiology section chief at NYU, said in a statement. After mild traumatic brain injury, “there is true structural injury to the brain, even though we don’t see much on routine clinical imaging. This means that patients who are symptomatic in the long-term after a concussion may have a biologic underpinning of their symptoms.”
Researchers specifically found that those who had sustained a mild-traumatic brain injury had less brain volume in regions linked with anxiety, memory and attention problems.
The bottom line here is that you can have a mild or moderate Traumatic Brain injury with long lasting debilitating symptoms and still have the same intelligence. You can have a severe traumatic brain injury with empirical radiological evidence and still maintain your intelligence. Brain injury does not equal lack of intelligence. A person’s intelligence is not a solid basis for deciding a person’s extent of disability after an injury.
The High IQ TBI (a blog which is worth the read about high IQ and TBI – this will take you to a different site)
Refrences:
1, 2, 3, 4, 5, 6, 7, 8, 9, 10, 11, 12, 13, 14, 15
Hey guys and gals…. Check out our latest story submitted by Tiffany McCullock – Survivor
Mental Illness and Brain Injury Are Not a Dual Diagnosis
https://youtu.be/y3-wLp9RyCs via @YouTube
Polytrauma / Trauma / Traumatic Brain Injury
Check out our Survivor Stories
We are working on some submitted stories right now. If you want to submit yours let us know. See our Story Submission Guide.
I really do not like the question “what do you do all day long?”
It differs so much from day to day and moment to moment that having a schedule is sometimes a curveball I miss catching; so there is no simple answer.
Before the wreck the answer was a lot more simple. Before the wreck it was wake up and get kids ready for school. Run errands, set appointments, pay bills, clean, organize, manage the household schedule, keep track of the budget…all this before I went to work for an 8-12+ hour shift. Come home check homework of kids, enjoy the family or deal with family drama (any day is a toss up with kids truth be told). Deal with all the things that comes with having a blended family, in-laws, and being a working mom and stepmom.
In my life before I would often be described as independent, bold, courageous, strong-willed, determined, a goody two-shoes, ethical, self-conscious yet perfectionistic, accomplish anything I set my mind to; a great multi-tasker, and adventurous.
THINGS I DID BEFORE: I was involved in my kids schools activities, field trips, PTO’s, on top of my full time work life. On top of all that Rick (my husband and I) managed to still do stuff with the kids and with each other away from the house. Though I have to tell you work was the main part of our lives as we both worked full time+. I loved to drive. Man did I love to drive. I even have my motorcycle endorsement (yep even used to own two of my own motorcycles before I met my husband). I loved going to the movies, the beach, museums, comedy shows, community events, carnivals, fairs, and other community events/fundraisers. I had a life that made me feel fulfilled and though stressful, exhausting, and full – nothing that a good night’s sleep, a warm cuddle, a payday, or a homemade dinner couldn’t fix. In some ways I believe I wore rose colored glasses and saw the potential and possibility everywhere. I also had a LOT of responsibility and my husband always referred to me as his “walking filing cabinet” (cuz I rarely forgot anything and knew what was going on when and where). I feel I always survived grief and stress with some kind of grace.
FAST FORWARD TO AFTER THE WRECK…..
A total cumulative time in the hospital as a patient 6+ months, literally 100’s of medical appointments, 4 surgeries, 100’s of therapy appointments, tons of labwork, and radiology galore. Near death experiences. Enormous and unwavering pain in ways I never imagined feeling such pain. A complete stripping of the body, soul, and mind through harsh realities about how the world works…..or rather doesn’t work if you are in a position to depend on it for your day to day survival.
Pain pain and more pain. The pain is so much that after a while you build a new tolerance to where the pain exists for so long that you almost don’t notice it because it is so much a part of you that you don’t remember the last time you didn’t have it. Then another surgery brings some relief and you get excited and become hopeful and then BAM something else pops up, or it flares up. All of a sudden, you wake up one day and realize that you are depressed, angry, about all that this “wreck” has seemingly taken from you. You find yourself so deeply exhausted, fatigued, and emotionally overloaded EVERY DAY that you want to cry but you have no tears….only sadness and a feeling of defeat. You look at yourself and you wonder what happened to that busy person who seemingly did everything. Where did she go? You entertain dark thoughts that you keep at bay because if you focused on them they would surely overtake you and swallow you up. Radical acceptance is painful you realize. Accepting that your new limitations, your memory problems, your scattered disorganized, lack of focus, emotionally mercurial self is your new normal. Suddenly you have all these rules about what you can and cannot do, why, when, and yet you keep pushing yourself anyway. At what point does the emotional overload – overload you to a point of no return? Every time I feel I cannot take any more…more is given to me by my body, or the universe that pushes me further down the rabbit hole.
The harsh reality and unspoken truths that no one really talks about as your healthcare provider….is that after extensive injuries is how the picture of your sex life changes dramatically; they don’t tell you that your social life, your work life, and your sense of self identity (unless you fight like hell to stay afloat) all changes; but these are real things that I think about.
Will I ever be able to return to a job again? Will I ever be able to think and function like I did before? Will I ever get my memory back? What does my future or life expectancy look like? How can I get value from the life I have now? How do I get away from living a life that I don’t truly get a sense of accomplishment from? How do I live a life for myself that has meaning, value, and matters? How do I not give up when the obstacles seem so impossible to overcome? How do I be for my kids, my husband, my family, what they need me to be – when I don’t even seem to be enough for myself? How much am I willing to do today which takes away from what I can do tomorrow.
I often think how would people describe me now? Brave, a miracle, survivor, pessimistic , emotional flooding, anxiety, impatient, forgetful, hurting, impatient, boring, scattered, obsessive and compulsive, lacking filters, insecure, intolerant, and riddled with panic, PTSD, irritability and feeling extreme waves of helplessness in this enormous sea of HOPE, love, and a desire to overcome, heal, and accomplish.
That me….the one who longs for normalcy….THAT woman seems further and further from my reach some days. Stricken with a deep-seated grief process as my childbearing days have surely come to an abrupt and non-consensual halt and the barren feeling and realization that having any more children would be dangerous to my body and would also require some kind of bodily performance that my body has seemed to have abandoned and I have been in deep grieving about. You know that song called “Someone that I used to know”…..yeah that is pretty much how I feel about sex right now. It’s how I feel about the ability to be a person who has to let go of the idea of bringing new life into the world. It’s also though how I feel about how I identify with myself as this person that exists now only in the shadows.
Here I am….and here is one more thing that the wreck seems to have stolen….. that level of intimacy from my marriage dented…that changed the dynamics of our relationship.
Take, take, take. These injuries just keep taking from me and my family. I need to change my thinking I tell myself and I do; I change my thinking. I need to change my direction I keep telling myself…so I focus on helping others going through this kind of struggle.
THINGS I DO NOW: Sleep, home therapy programs, medical appointments, research my medical stuff, blog to help myself and others with Polytrauma and TBI, sleep, cope, be the best mom and wife I can with where I am at right now (which is not even close to where I want to be), more activities as my body will allow, and did I mention sleep?
Knowing I HAVE to go in a direction of mind and body positivity to stay motivated (huh…what is motivation?) and having no clue how to get there is very lonely and makes me feel lost sometimes.
I have to be kind to myself in order to move on. Dancing through the dynamics that each day brings is sometimes seemingly impossible. Yet somehow, someway between each excrutiating headache or spasm….I scrounge, pillage and plunder and find a wee bit more courage to get me through the day.
Defeat, Depression, cycling grief and a dedicated struggle to excel and never give up – the unspoken truth of emotional overload from a Polytrauma.
 not own it as my own, but rather something I experienced.
not own it as my own, but rather something I experienced. may be thinking wow thanks for sharing information I didn’t need to know. Why does this matter to me as a reader? Good question!!!
may be thinking wow thanks for sharing information I didn’t need to know. Why does this matter to me as a reader? Good question!!!
Please comment below and share this post with someone. Let’s spread the word and bring awareness.
Just wanted to post that we have completed another page on our Website here to assist you in getting some answers.
I just want to note that I have been chronically anemic AND have had continually low Vitamin D counts since the wreck. In fact while hospitalized within those 3.5 months after the wreck, my Vitamin D was less than >1 (not even readable) – crazy huh?
I have been on lots of Vitamin D supplements since the wreck too – D2 D3 and Calcium+D….so Deficiency Def Trauma related!!!
Give a read, make a comment, and share…
Inquiring Minds want to know: What were your injuries?
I always wonder if they want a full answer. Sometimes it seems too much to talk about so I just say “polytrauma”. Sometimes this is sufficient. If not, it will lead to more questions that are almost always more specific.
Believe it or not I finally have most of this list memorized now after 3 years. However, I still always leave something out when talking to someone and trying to determine what to tell what specialist or what is important to mention or what wasn’t….this was not only overwhelming but impossible.
My family had kept track of injuries as they were discovered and this is their list in addition to mine once we started combining them and matching them with Medical reports we had. These are the injuries from the 2014 wreck in chronological order of discovery. The list is great because I just add to it as things are discovered and then just provide the list to my providers when I see them. It also saves time during the visits from those ultra short times which are never long enough for a polytrauma patient.
Yes I know it is my personal medical information I am putting out here, yet my bravery (or stupidity perhaps) to so openly share all this has helped me learn valuable information from others to get properly treated and helped me acquire a higher index of awareness about my body and the care that is or is not given to it.
If you see something here that pertains to something you have questions about maybe I can answer the questions and help in some small way. All in all, recovery and rehabilitation is a work in progress. Not something all diagnosed in an Emergency Room or Ambulance. Things are always unknown or missed there.

Arnold Chiari Malformation is definitely a tongue twister. The other name that it goes by, is “Syringomyelia”, and that’s not any easier. It is also something that I was likely born with. Sometimes type I or II are an intra-uterine abnormality in which the tonsils of the brain become herniated and the “foramen magnum is […]
Hello folks. After much consideration it was decided that HOPE TBI should have it’s own Twitter affiliation that wasn’t hooked to my personal Twitter account. Just figured not everyone would be interested in all the personal tweets that did not necessarily have anything to do with the goal of the website/blog.
So while it says joined Twitter recently….we have actually been tweeting for a while…just making it more user friendly.
Come join us and follow our website and our Twitter #hope_tbi
Awesome news!! Page translation now available on our website. Now available in 103 languages. See sidebar at right of page and then click dropdown and click which language you want the page translated to.
One step closer to global awareness!!! Yay!!!
 I have been thinking about what to write today, January 4, 2017 for about a month now. Here I sit trying to think of how to form the words that swim in my mind and express them in a way that makes sense to anyone else but me.
I have been thinking about what to write today, January 4, 2017 for about a month now. Here I sit trying to think of how to form the words that swim in my mind and express them in a way that makes sense to anyone else but me.
Today marks an important landmark. A valuable piece of history worth honoring. Today marks the 3rd year Re-Birthday Anniversary for Austin (my son) and I since the wreck where I became a survivor of a Polytrauma and TBI and my son seemed to have escaped physically unscathed by traumatized still the same. We continue our journey still today. We both have come so far in 3 years. I myself have met many goals, yet miles to go before I sleep….soundly that is *smiles*.
It has been an extraordinarily long journey through this whole recovery process….and still is. I needed an outlet. I needed to learn, to teach others what I had learned the hard way so they didn’t have to work so hard, to understand myself, to hopefully allows me to heal.
This page at posthope is strictly my medical story as it has unfolded and continues to unfold. It is fantastic and I need to make an effort to get here more often. I went through a round of blah there for a while.
I know though that I love helping people, I am just not able to do it in the way that I used to. I started a personal blog, which was so disjointed I couldn’t find anything when I wanted to, so with the help of my tech savvy husband he taught me how to use a very user friendly program where we changed the blog to a website so it was more organized. This was very helpful and allowed me to find things easier. The website is a work in progress that allows me to heal and help others. I want to help other survivors cope, or caregivers/healthcare providers maybe try to understand what it has been like for our family so they do not feel so alone, or so they can develop different ways of doing things, of helping, of surviving.
HOPE was a word my mom hung up for me when I was in the hospital shortly after the wreck. I found myself so focused on that word that sometimes, all I could do was stare at it to get me through the day. I am unaware of the time frame that was wrapped around this. However, my memory makes it feel like it was a long time.
As time progressed it became the word I would include in my meditations, my prayers, and my self-talk to keep moving forward and never give up. To me HOPE became a symbol and acronym for “Hold On – Pain Ends”. The pain never seemed to end though and so this seemed completely unrealistic to me and not something I could honestly uphold. I struggled to think of something that would help me remember to never give up HOPE.
I also wanted to have HOPE represent my experience with all the medical providers, insurance processes, and developments and knowledge we had either been blessed or seemingly cursed with. I wanted to represent my journey as an ongoing recovery process, as that is exactly what it is. Days led to weeks, weeks to months and soon it came to me one day as I was in enormous pain that some of these providers were actually trying to help me gain my independence back and I was fighting full force to gain back what I felt I had lost. I needed so badly to excel…to move forward and move on with my life.
So was created ” HOPE TBI”
Help One Person Excel – To Be Independent
Hence this site was innocently started, and continues to evolve as I continue to as well. I also now share other people’s stories as well as it is very healing to have a voice in some form and not feel so alone in a situation where you are surely to lose life as you once knew it….lose family….lose friends….as you adjust to your “new Normal”. The folks that do decide to stick around…they feel alone too. Their commitment to you causes their supports to move on with life while they remain with you PERPETUALLY FROZEN (look for this as a new post title soon).
This existence is not for the faint of heart. It is not for the weak. It is not easy. I feel gratitude though for my life. Grief and gratitude are constant bedfellows that have learned to coincide with each other.
Today I am reminded to reflect on not only all that was, but all that is, and HOPE for all that will be. January 4, 2014 I was born again. No, not in a religious sense. However, I continue to experience a metamorphosis of epic proportions. I continue to strive to embrace my “new normals” and function to the highest levels possible. Thank you to all who have stood by me, believed in me and advocated for me. Thank you for those who cared for myself, for my son, for the other driver (Greta) and made waking up each day seem possible.

The complexity of Change and how it affects my new normal. I was inspired to write about this for several reasons. I may totally suck at expressing what is in my head here on paper or this screen, but here goes….
It is not all inclusive of every situation in my life, how I see people outside of me in general, how I exist inside myself, or how I handle stress overall in every situation….but it comes pretty darn close to kind of manifesting a picture of an inner struggle that is life as I know it now and my desire to overcome, understand myself, and help others who might experience this after trauma not feel so alone.
I don’t handle “change” as gracefully as I used to. Change in general I have gotten pretty okay with, as a genral rule, if done in advance with plenty of warning or notice (unless it is something time sensitive and important then it is instant anxiety). However I have come to notice that the little stuff…stuff that probably shouldnt even bother me, or wouldnt have before the wreck…does now. Though that can be inconsistent too.
I know…I am consistently inconsistent. Imagine how horrible this inconsistency is for the person going through it who now thrives better with lists, strategies, consistency….or order.
Sometimes last minute changes leave me feeling just gloomy, depressed, and sad. Sad is not my normal emotion with this. Mostly it is being irritated …okay…highly irritable….when things change. Following through the plan has become very important to my daily feeling of a successful day.
I feel I cannot leave the house and feel calm without my to do list (this can be mental or written…though more often it is written). This list will be in a specific order too. If things are done out of order, I get irritated or frustrated and the chance I forget something increases.
Small things/changes that should truly be insignificant in the day that involves me personally, just are not that small to me…they can be monstrously huge in my perception at that time…in that instant.
I cannot explain the sheer anxiety that those little changes cause me now. I used to not mind them so much before the wreck…I would definitely adjust quicker or maybe I just wasn’t aware of them at all…things that just cause hiccoughs throughout a normal day (whether they are small or large). Things that wouldnt slow me down…but now can seemingly paralyze me.
Now though…it is so important to stick to the plan.
If I analyze something afterwards…sometimes I realize it shouldn’t bother me or that I am being ridiculous..or how I should have handled it differently….yet I plan my day based on lists and when those lists change it messes up my day….it throws me off course.
I get that morose feeling when I forget things….it is usually appointments I forget and conversations…important things I am sure I will remember…it is humiliating. I make lots of lists. It kills the mood if I forget them. I am still working on adjusting to that part.
I have come to somewhat have a sense of humor about all this (this depends on what kind of brain day I am having for sure). Some days are better than others.
I recently had someone express it sounded like OCD or impulsivity.
I guess I never recognized it as an OCD thing or being impulsive. I have never had OCD in my life or been diagnosed with that ….maybe it is OCD or not OCD at all. I just know it is inconvenient.
Sometimes if I get all worked up about something (positive or negative), get prepared for it, have all my notes ready, have all the pieces in place and it gets cancelled, or I am late and it gets cancelled, or it ran over and I am late to othet things….that is a real problem for me.
If I am depending on a certain schedule that day and then realize too late that I have looked at the wrong day on the calendar….I sink into embarrassment and self-defeat and dark places inside myself. This can also manifest itself as a sheer and utter sadness, or complete internal rage. I cannot tell you the times I have missed an appointment because I forgot about it (even if I looked at the planner 2-3 hours before that), or the opposite… shown up to an appointment early, proud of myself, to be told I dont have one that day. I have gotten better about checking my planner and my phone to compare dates and times, before arguing with the receptionist. Dealing with the feelings after are another story. Those emotions can very from feeling relief (if I was running late anyway and now get a second chance) to feeling confused and crazy ( if I am really quite sure about the day, the facts, and was feeling confident).
My husband will often accuse me of micromanaging his driving and trying to control his driving and what we do with the day. I assure him that is not it at all or what is going through my head. It is not about HIM. It is about ME. For example, there is a certain way I go to specific places. If he goes a different way it throws me off and then I get anxiety about being late. (I DESPISE being late to anything), or I feel a twinge of irritability that I have to silently or not so silently quell. Also if I gasp or make any sounds at all he is like…”knock it off I’m a good driver Caren when have I ever been in an accident?” I tell him I am and was a good driver too yet accidents still happen. I tell him if something is scary to me. I tell him if something is freaking me out….when things seem enhanced around me and magnified…sometimes just taking an exit ramp can feel like we are tipping over on our side and the wheels have left the ground and enormous fear overwhelms me and I have a deathgrip on whatever I can hold onto and beg him to slow down (even though the wheels dont leave the ground). Even if I look at the speedometer and can “see” we are going an appropriate speed….it feels so different. He doesnt understand that about me now and it has created opportunities for even the kids to get in on comments to mom about whatever is going on or join in on making jokes about it. Other days he can take the same exit faster and it doesnt bother me a bit.
I go one of two ways with anxiety. It is also depending on what kind of a “brain” moment I am in. What I call “enhanced” or “tunnel vision” with my anxiety. Enhanced means that suddenly colors are brighter, lights are brighter, sounds are louder, I notice every movement around us, its intensity in minute ways. This can last moments to all day. Tunnel vision is like when a car is sliding towards me and all I can see is that car and all the peripheral stuff disappears until the car stops sliding. The sliding (whether it is continued or stopped), even if a slight shift in the lane or a flat out across the intersection slide by that car appears greater and larger….it triggers these deep emotions that are just automatic and overwhelming, and often debilitating emotionally, mentally, and sometimes physically. (That is when I feel overstimulated or burst into tears, and it’s time to go home NOW, or an unavoidable nap ensues, .or a meltdown…depending on how intense the situation is).
I then get annoyed or irritable because I am genuinely upset or scared in that moment in the vehicle. I literally feel like something horrific is about to happen or has happened. He tries to joke with me to make me laugh…I have learned to try to go along with that….but sometimes I just start crying instead and not even mean to…then I am mad at myself. It’s not his fault I feel this way. So being mad at him in those moments is not helpful. So I am always analyzing my feelings, my reactions, my words. Sometimes not until after the fact….which can cause some tense moments.
Another example is I am getting ready to leave the house. I have to do things in a certain way now. Okay I think Bag, notebook, pen, planner, phone, charger, wallet, cane, and keys. Sometimes keys comes first but that is the order . Now if one of the kids, or my husband, or anyone, or a phone call interupt that mental walkthrough of the list, and I don’t start the list over…. then I ALWAYS forget something and if its the planner or the phone I am really screwed and it ruins everything about the day if I end up out there without them. I really depend on all those things. Even if I dont use them all on my outing just KNOWING they are with me and functional matters.
Change sometimes comes with complex anxiety. Sometimes it does not. Little things can appear like big things and big things either matter or they don’t. Functioning despite all those nuances is the key. Sometimes finding the right key to all those “locks” is the challenge. I cannot explain it beyond that.
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
https://hopetbi.com/reviews-and-testimonials/
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
 ADVOCACY:
ADVOCACY:
I feel it is imperative that I voice my strong and unequivocal support for the NO FAULT system and voice that I speak about this system from personal experience….not just opinion from a desk somewhere trying to increase our financial “bottom line” (like insurance companies want to do) without knowing or understanding the ripple affect of taking this much needed program away or altering it for the patients whose lives literally depend on this system being in place.
No Medical Limits For Life (no Financial Caps on reasonable and necessary Care for injuries related to wreck):
I just want to say that here we are almost 3 years later and we are still discovering injuries acquired from the wreck. These would not have been found and treated if it were not for the current No Fault System and my disabilities would have been much more extensive.
I never would have been able to get out of the wheelchair, or have the majority of the use back in my right arm without the lifesaving reconstructive surgeries in MN by Dr. Peter Cole. I wouldn’t have gotten the life saving Rib Surgery here locally by an Orthopedic Surgeon to plate ribs 5,6,7,8,9,and 10. I wouldn’t have had access to all the Specialists I have see or been referred to.
I wouldn’t have received the extensive and ongoing Physical Therapy, Occupational Therapy, Speech Therapy and Counseling needed to help me Rehabilitate.
I would not have been given the majority of the radiology (Xrays, CT Scan, MRI’s, etc), EMG’s, EEG, and other testing; the Dental Repairs, the Vision Therapy, the Audiology Testing and Follow-Up Care, Case Management, etc.
I would not have been given Recreational Therapy and Vocational Therapy to help me return to some form of a quality of life.
Household Services (Replacement Services) and Attendant Care:
Without these things in place I would not have been able to come home to a hospital bed to be near my children and my family after NeuroRehab. I was able to be cared for in my home where there was less chance for infection, higher rate of healing ability in a real world environment, by my family or caregiver of my choice. I was more and more appreciative as time went on and it allowed me to be near my husband and my children and them near me. A cap on Attendant Care would be Catastrophic for any Survivor. There were some weeks that I needed 24 hour care 7 days a week. Other weeks 16 hours of care then 14 then 10 then 6 then 4 hours per day seven days per week. This continually varied based on what was going on with me. I often used several hours a day 7 days per week after each major surgery.
Without this system in place. I know for a fact, without a doubt, I would be dead 2.5 years ago now due to the Polytruma I sustained which included multiple orthopedic injuries and multi-system involvement.
There are a lot of things that have been resolved. There are some injuries I will have for life (like my back injuries, hardware in my body that may need replaced later in life, and various other injuries being cared for, etc. I wake up every day….grateful for my life. Grateful for the NO FAULT system here in Michigan.
I am the poster child of sorts about how the success of the NO FAULT system can work when given the care needed. I will also add that if the insurance company did not fight this benefit so much, it would have cost less over time as I would have received recommended treatments in a more timely manner and not have had to suffer the debilitating chronic pain of unhealed fractures, nerve damage due to delayed treatment, and exacerbation of other disabilities for the duration of time that I did.
I will also say that there needs to be an educational process in place for families and patients from the beginning on what is available and how to fill out paperwork properly etc. This would eliminate a lot of challenges that present themselves by learning things the hard way.
I can say that I didn’t even know what NO FAULT insurance was until falling victim to this catastrophy and needing what NO FAULT provides to either live or die.
So What is Auto NO FAULT? There are several states that have it….Michigan is the most comprehensive.
A Michigan no-fault policy provides unlimited medical and rehabilitation benefits. It provides wage loss benefits for up to three years, and $20 per day for replacement services if you are injured in an auto accident, regardless of fault. In exchange for these benefits, Michigan motorists gave up the right to sue in auto accidents except when someone is killed
or very seriously injured. Because of this, disputes over who was at-fault in an accident will not hold up payment of medical bills. Michigan is unique in that damage to vehicles also falls under the no-fault system. This, too, saves time and money in claims payment. Michigan drivers must buy collision and/or comprehensive insurance to cover damage to
their own car.
The Michigan Catastrophic Claim Association (MCCA) was established in 1978. The MCCA
pays for claims paid by an insurer that exceed a certain amount. All insurers that sell auto insurance in Michigan must pay the MCCA an annual fee for each vehicle insured. That fee is known as the MCCA assessment, and is passed on in whole or in part to the policyholders.
The Basic No-Fault Policy Has Three Parts:
Personal Injury Protection (PIP) -If you are hurt in an auto accident, this part of your no-fault policy will pay all of your medical costs. It will also pay up to 85% of the income
you would have earned if you had not been hurt, for up to three years.
Property Protection (PPI) No-fault will pay up to $1 million for damage your car does in Michigan to other people’s property, such as buildings and fences. It will also pay for damage your car does to another person’s properly parked vehicle. It does not pay for any other damage to cars.
Residual Bodily Injury and Property Damage Liability Insurance (BI/PD)
What is an Assigned Claim?
The State of Michigan established the Michigan Assigned Claims program in 1973 to provide assistance to people injured in an accident involving a motor vehicle, when there is no automobile insurance available.
The Secretary of State managed the Assigned Claims program until December 17, 2012, when it transitioned to the Michigan Automobile Insurance Placement Facility.
The state of Michigan provides a safety net of insurance coverage for no-fault (PIP) benefits in situations where a person is involved in a car accident, but there is no insurance company available to provide no-fault benefits.
The name of the safety net is an organization called the Michigan Automobile Insurance Placement Facility (MAIPF), formerly known as the Michigan Assigned Claims Facility. The Michigan Automobile Insurance Placement Facility (MAIPF) is considered the insurance company of last resort.
The Michigan Automobile Insurance Placement Facility (MAIPF) administers the Michigan Assigned Claims Plan, which sets out the procedures for ensuring that Michigan No Fault benefits are provided to uninsured auto accident victims.
The Michigan Automobile Insurance Placement Facility (MAIPF) does not apply to a person driving an uninsured car that is owned. However, if an individual who doesn’t have auto no-fault insurance is injured in a car accident in a non-owned vehicle, and if there is no other insurance company of higher priority, then the Michigan Automobile Insurance Placement Facility (MAIPF) would provide payment of benefits.
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
https://hopetbi.com/reviews-and-testimonials/
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
 My life has been enormously eventful since my last post. There is a lot to catch you all up on. Many days have passed. I sat here staring at this screen trying to decide what to write, how to tell what I was going through, what I was feeling, thinking, experiencing. The words just weren’t there. It felt redundant and repetitive.
My life has been enormously eventful since my last post. There is a lot to catch you all up on. Many days have passed. I sat here staring at this screen trying to decide what to write, how to tell what I was going through, what I was feeling, thinking, experiencing. The words just weren’t there. It felt redundant and repetitive.
I thought…really Caren, who really reads this anyways? What is the purpose of writing and posting, and keeping this going. It is something I pondered for a long time. I mean here I am back from the brink of death, more than once even and what can I offer my family, my friends, those who follow these posts, those who may come here to see how things are going? I can pretend to be positive and progressive and optimistic…but the reality is – I have been depressed. Feeling overwhelmed. Grateful, yet in many ways disappointed. Yet, in other ways completely neutral perhaps even apathetic.
What was this numb feeling? This path that took me down a side road with various cul de sacs that made me feel like I was disappearing within myself. The reality that with improvements and increased abilities which are uplifting and exciting….there also comes the awareness that once I feel I get to the end of one dead end road I am forced to turn around and head back out to the main road of my life and face the realities of my limitations and seeming roadblocks that prevent me from moving on.
This. This here is where I find myself drawn back to. Writing, sharing, purging. Giving what I have learned to the Universe beyond me. Hoping I make a difference in some small way.
Each day is a reflection of improvement and as I look in the rearview mirror of my body, I see the rubble. I feel the dings and dents it has left on me. I have been rebuilt in a lot of ways. Though I have a few misses here and there and everywhere – I am also looking at the road ahead and where it can take me. I try to avoid those emotional cul de sacs that pull me off of my path in various ways.
So here I am. Facing the inevitable. Facing my own mortality with each spasm, bump and grind. Facing the future with uncertainty and grateful….ultimately….that I am here to continue this journey.
This is my life. My new normals. Yet at which point do they stop being “new normals” and just are who I have been becoming the last nearly 3 years. This is my life. My life is not based on imaginary twists and turns. My life is based on a True Story. My life…the ultimate Cul De Sac.
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
https://hopetbi.com/reviews-and-testimonials/
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
Hello there. I am a polytrauma and TBI survivor. I acquired mine from a wreck (head on collision) where my seatbelt failed and I was ejected (see Frequently Asked Questions page for more details).
I for a long time, felt it wasn’t important to “show” a picture of who I was. I have gotten lots of requests for this though. I realize people want to see a “real” person. I wanted and still want… the site to be something that could be relatable regardless of what a person looks like….because after all…TBI is often invisible. So are most bodily trauma’s once the bones heal. Yet this is NOT the end of the healing process.
This website is a growing passion for me with the more I advocate for myself, learn about myself, and learn about others experiences. This website is an outlet for my continued healing, rehabilitation processes, and a way to share what I have learned with others. Helping One Person Excel I truly believe…begins with who I see in the mirror each day – Me.
To Be Independent is always the goal….yet that comes with a lot of dimensions and levels of intricate obstacles. I hope that you find something in the pages of this site that help you, or someone you know.
If you’d like to share your story, or offer a guest blogging post …that would be amazing. Your story matters. Are you a Survivor, Caregiver, Family Member, Healthcare Provider, Friend, Employer, Co-worker? Whether the person is living or deceased…their story still matters.
Feel free to ask me questions in comments below or in email at hopetbi4ever@gmail.com I will answer as honestly and as directly as possible.
I am hurting so much tonight. I had 2 Baclofen to help with the super incredible muscle spasms which seem to be happening more and more and with an exhuberant intensity. My head has been rocking out some pretty intense headaches and sometimes it feels like my head will pop off my shoulders from the throbbing and crushing feeling that comes with them.
Finished my first day on a new Thyroid medication. Hopefully this will get my system back to pre-wreck status….its taken me over 2 months to get this since initially prescribed. Hope beyond hope at this point.
If I had tears to shed I dont think I would ever stop crying sometimes. Sometimes those tears flow at the most awkward times. Then other times, like now, when it feels I SHOULD be crying…the tears are nowhere to be found…almost lime they arent capable of flowing. I am glad for my life. However the pain in general, the nerve pain, the spasms…..its just damn exhausting. I mean seriously, it wears me out and then I am rocking in bed while laying down until I can fall asleep and escape that pain for a little while. Too tjred to sleep. Brain racing from thought to thought…….ok….gonna try and catch some zzz’s.will catch up this weekend with you folks.
https://m.youtube.com/watch?v=yP1iKqcGfD8
What is a typical day? I used to be able to tell you this until January 4, 2014. That is when everything that became typical about my life, my health, my existence, became consistently ATYPICAL.
I feel like a Turtle walking around in a hollowed out shell moving slowly and hoping I can make it far enough and long enough to get to where it is I am heading. Where is it I am heading? That is a great question. I often forget the answer as I am heading in so many directions at once on so many different levels….even if I am sitting perfectly still and quiet.
HOPE can only get you so far. I try to hold myself back from the dark abyss of resentment and emotion that try to pull me over that cliff of depression that reminds me of all my limitations, injuries, pain, and I feel robbed. I am robbed not only of my function, endurance, memories, peace, and joy. I feel robbed of opportunities, freedoms, laughter, and just simple existence.
I guess all my new normals that are no longer really new….yet new enough to feel like fresh wounds with salt dripped into them on a daily basis are who I am now.
I wake up sometimes more tired than when I went to bed. Sometimes I wake up ready to conquer the world only to be exhausted by the time I muster enough energy to actually get dressed or to take a shower. Then other days I am blessed with a full day of accomplishment. I actually get out of the house and make my way through the world ignoring all the struggles that seek to slow me down (pain, confusion, forgetfulness, dashed joy, excitement, fatigue, bathroom breaks, sadness, and the seeming lack of motivation for life all at the same time).
What is a typical day? The only typical day is that I know I will face…..is a mountain of uncertainty. Will I have an accident? Will I forget something important? Will I be late? Will I remember to use my words and respond instead of just reacting emotionally? Will I get everything done I have put on the list? Where is the list? Did I make a list? Where is my planner? Where is my phone? Where is my charger? Where are my shoes? okay let’s go….oh crap, I forgot to put on pants. Okay pants on now…wait where did I put my bag. Do I have my planner, my phone, a pen? My charger….wait…gotta pee…okay flush toilet wash hands phone rings get planner talk on phone …kids talking “mom mom mom” wave them away finish on phone….head spinning I have everything right? Feeling irritable already. Oh no I read the time wrong now I am super late. I totally need help here feel like I am drowning. Feeling flooded and overwhelmed or not just yet but feel it coming on. Try to avoid it. Deep breathing, Relax. Husband asks if he can help or he doesnt ….kids a distraction or they aren’t. Okay let’s go…wait I need to have water with me. Man am I thirsty. I have to remember to take my meds. Okay do I need meds now? What is my pain level? Lets skip pain meds I can do it. Oh my gosh what was I thinking? I have to be somewhere but I can’t put my finger on it. What was I doing? Where am I going…I don’t remember. I look at the white dry erase board what is today? I cannot remember what day it is. Look at phone. OH okay…I have it now. Oh no I got my days wrong I don’t have appointment today….wait yes I do I looked at the wrong day. Okay lets go. What am I forgetting? It feels like I am forgetting something. Where’s my list of questions for the provider? Where is my List I know I had a list….oh that’s right I forgot to do the list because I fell asleep. Okay out the door, let’s go. Get in van, let’s go…. pat pockets for phone; crap – muscle spasm; damn this headache, I will be fine. I feel like vomiting. I am a passenger n vehicle and moving now….crap I left my bag at home with my planner. Panic what do I do? Focus, look at phone distract yourself.  You are safe. It’s okay. No planner can’t go back or will be late. Have to have planner MUST have planner. Panic ensues or it doesn’t. Go get planner or skip it if running behind which is often even if ready to go early. Leave without planner day ruined. If leave without phone feel lost and alone day ruined. I have alarm reminders and email and ways to communicate with people if I need help with something. In vehicle “no don’t hit us” *car swerves in our lane or slams on their brakes or gets too close to us”. Oh my gosh I cannot wait to get home. Okay I can do this. Quit wimping out Caren push push push. You can do it. Not so bad right….oh crap another muscle spasm. I am really hurting today or not really hurting as much. I am happy but so worn out and I haven’t even done anything yet; or I feel great and then someone zooms in front of us or we see someone almost wreck or act crazy…instant fear and nap time to escape brain shuts down I am done. NO! I have too much to do. NO sleeping. I am sorry I didn’t mean to fall asleep. Are we there yet? Thank God I did it. I knew I could do it. Why can’t I get anything right? I hate forgetting so much. Slow down. I want to go home. I feel like crying every little sound is annoying. Talking is annoying, the wind when the windows are down is annoying. Man my back hurts, my neck is killing me. Wow my shoulder feels better since surgery now…I love those people. I think I am going to cry I am so happy my shoulder is getting better. Oh my gosh how will I get through this day. I am already running low on energy. Wait…where’s the bathroom. I have to go RIGHT NOW….great a piddle I hope noone can tell. Did I bring extra underwear? Oh yes I did…. get relief or no I didn’t shame lingers. Good morning world I love you or I can’t stand any of you at this moment and I don’t know why. Shhhhhhh not so loud the lights hurt my eyes. I am okay. What? You want me to answer what question? Yes I am okay. Why are you staring. I don’t care if you stare I am proud to be alive or man I can’t get away from the pain to I just can’t stay awake I am sorry I AM DONE…my brain is done. Can we go home now? Think Think Think what was I doing? Oh That’s right, smile act normal. Stay quiet or not so much. Wash rinse repeat every day.
You are safe. It’s okay. No planner can’t go back or will be late. Have to have planner MUST have planner. Panic ensues or it doesn’t. Go get planner or skip it if running behind which is often even if ready to go early. Leave without planner day ruined. If leave without phone feel lost and alone day ruined. I have alarm reminders and email and ways to communicate with people if I need help with something. In vehicle “no don’t hit us” *car swerves in our lane or slams on their brakes or gets too close to us”. Oh my gosh I cannot wait to get home. Okay I can do this. Quit wimping out Caren push push push. You can do it. Not so bad right….oh crap another muscle spasm. I am really hurting today or not really hurting as much. I am happy but so worn out and I haven’t even done anything yet; or I feel great and then someone zooms in front of us or we see someone almost wreck or act crazy…instant fear and nap time to escape brain shuts down I am done. NO! I have too much to do. NO sleeping. I am sorry I didn’t mean to fall asleep. Are we there yet? Thank God I did it. I knew I could do it. Why can’t I get anything right? I hate forgetting so much. Slow down. I want to go home. I feel like crying every little sound is annoying. Talking is annoying, the wind when the windows are down is annoying. Man my back hurts, my neck is killing me. Wow my shoulder feels better since surgery now…I love those people. I think I am going to cry I am so happy my shoulder is getting better. Oh my gosh how will I get through this day. I am already running low on energy. Wait…where’s the bathroom. I have to go RIGHT NOW….great a piddle I hope noone can tell. Did I bring extra underwear? Oh yes I did…. get relief or no I didn’t shame lingers. Good morning world I love you or I can’t stand any of you at this moment and I don’t know why. Shhhhhhh not so loud the lights hurt my eyes. I am okay. What? You want me to answer what question? Yes I am okay. Why are you staring. I don’t care if you stare I am proud to be alive or man I can’t get away from the pain to I just can’t stay awake I am sorry I AM DONE…my brain is done. Can we go home now? Think Think Think what was I doing? Oh That’s right, smile act normal. Stay quiet or not so much. Wash rinse repeat every day.
Some days are a blessing. Calm quiet, no appointments, no need to think, no need to go anywhere or do anything. Time to sleep to recover from the days I was just existing.
 So I focus as much as I can on researching myself learning about how to get my quality of life back leaving no stone unturned. Yet some days defeat wins a round and I cannot even get out of bed to get dressed. Sometimes I am hurting so bad the tears flow and I cannot stop them hard as I might.
So I focus as much as I can on researching myself learning about how to get my quality of life back leaving no stone unturned. Yet some days defeat wins a round and I cannot even get out of bed to get dressed. Sometimes I am hurting so bad the tears flow and I cannot stop them hard as I might.
I feel defensive like I have to try and explain why I am late, moving slowly, hurting, forgetful, struggling in some parts of my day and not others, yet there is nothing to defend. I feel like I have to explain everything as I go to educate others when they just don’t understand. That is not my job. What is a short answer? I don’t even know really anymore. So I just say it’s a good day to be alive.
I detest being late. I detest even more forgetting things. Important things. Conversations, appointments, easy things, important things. Why can I remember some things and not others. Why are there so many gaps. It is what it is I keep telling myself. Apply your strategies Caren. I can be vicious with my words and equally as generous. I can be brave and fierce and face the pain or I can crumble like a wadded up piece of paper. The only thing that is consistent is my inconsistencies.
No, it’s not fair, it’s not productive, it’s not ideal. It’s not easy. Yet it is an opportunity to appreciate life in a different way and I am constantly caught between never giving up hope and just not giving a crap anymore. Sometimes the fight to recovery is just so painful and long and lonely and utterly draining. Sometimes you just feel like damaged goods overwhelmed by trying to not forget all the things that are important to make it through each day. Sometimes each moment. Then it passes and all is well with the world again…for just a little while. I talk yet noone hears me. I listen but their mouth moves and I don’t hear their words. Never the same. Nothing can explain it. A different language or no talking at all.
The journey on these dusty roads are not without exhaustive effort. Hard as you try to keep  from getting dirty you are bound to have accidents, forget important things and be late to things. If there is one lesson to be learned in all of this – it is to face your fears and do not let them eat you alive. Forgive yourself for forgetting and remember that you know you better than anyone else. Sometimes invisible effort. Sometimes invisible limitations. Sometimes invisible pain is more painful than the fractures that resist healing and like those fractures need added support. My goal is to pave those dusty roads with healthy recovery and continue to use tools to survive with. I am not stupid by far, just different than what I once was. So I will mosey on along like the turtle….. slow…. to control the pain and thrashing muscle groups. Slow so I respond and not react. Slow so I can gather my thoughts. Slow so I can hold on to what I need and release what is not effective. Slow and steady wins the race. Isn’t that the ending?
from getting dirty you are bound to have accidents, forget important things and be late to things. If there is one lesson to be learned in all of this – it is to face your fears and do not let them eat you alive. Forgive yourself for forgetting and remember that you know you better than anyone else. Sometimes invisible effort. Sometimes invisible limitations. Sometimes invisible pain is more painful than the fractures that resist healing and like those fractures need added support. My goal is to pave those dusty roads with healthy recovery and continue to use tools to survive with. I am not stupid by far, just different than what I once was. So I will mosey on along like the turtle….. slow…. to control the pain and thrashing muscle groups. Slow so I respond and not react. Slow so I can gather my thoughts. Slow so I can hold on to what I need and release what is not effective. Slow and steady wins the race. Isn’t that the ending?
Damaged goods? I say yes. Destroyed? I say no. Fight or flight? Let’s get those wings!
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
https://hopetbi.com/reviews-and-testimonials/
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
https://hopetbi.com/reviews-and-testimonials/
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
Well. Good morning. Here I am the day after the 4th of July -Independence Day. This day holds special meaning for me every year because what it represents.
In the United States, this date commemorates the adoption of the Declararion of Independence on July 4, 1776 by the Continental Congress making a declaration that the 13 colonies regarded themselves as a new nation, and no longer part of the British empire. They declared themselves as The United States of America.
I have always associated this time of celebration as a time to remember all that was accomplished during that era. I also associate this time with fireworks, freedom, grilled food, potato salad, red white and blue clothing or apparel, picnics, and giving focused homage to our flag.
Well, each year since the wreck has been a bit different for me around this holiday.
In Jul 2014 I was at home in a hospital bed after 3 months in the hospital….so…6 months post wreck and all I really remember from that time is lots of sleeping, lots of pain, and the last time we were together as a whole family with almost all the kids….and did I mention LOTS of pain and not being able to breathe well. It was a rough time. Just the sound of fireworks scared me. Suddenly my beloved holiday was somehow tarnished and I had been forced beyond my control in losing my Independence.
July 2015 I forced myself to go see fireworks with the family…mostly for the kids’ sake. This ultimately was great for the kids, but I paid dearly for it with my health. I did not react well internally with ALL the people….it was too crowded, it was too noisy, and the loud exploding booms which I had for my whole life associated with happiness….now frightened me at a core level. I was hurting, it was hard to “look up” and I literally was biding my time in anticipation of getting back home where it was quiet (at least in my room) and safe.
July 2016. I have learned my limits and am learning that even some of our family traditions have changed in some ways as part of our family’s new normals as well. This year…I decided to stay home. Away from the crowds, the noise, just everything. I don’t regret it and was glad to hear about the crowd craziness I missed. Next year.. I can try again.
Anywayyyyyyy…
I survived 3 pretty intense orthopedic reconstructive surgeries in the last 6 months. I feel like I have been given a very special gift….Independence. So my rehabilitation journey continues and I am learning to say no thanks on behalf of me…
So for all of you out there struggling to get through each day….for all your mini accomplishments and for each breath you are able to take…..take care of your health…even if it means breaking traditions or doing them differently. You are a new nation with your new normals….
Happy Independence Day!!!
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
https://hopetbi.com/reviews-and-testimonials/
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
Cinco De Mayo (May 5th) is the date that is observed to commemorate the Mexican Army’s unlikely victory over French forces at the Battle of Puebla on May 5, 1862.
Much like Cinco De Mayo….my recovery and rehabilitation processes have had numerous UNLIKELY VICTORIES!
So it is ironic, and while tragic – also beautiful that my proposed final surgery on my shoulder/scapula/Acromion process was on May 5, 2016. This was the surgery that would also give me MY independence…..from an orthopedic (arm/shoulder) perspective anyway.
Now…to just wait until my follow-up appointment on June 1st to clear me for the Physical Therapy Regimen (exciting stuff).
I continue to be in awe of Regions Hospital and Health Partners system of patient focused care there in St. Paul, Minnesota. Perhaps because my providers there have been so instrumental in being so responsive and progressive in numerous aspects of my care, and continue to be.
On May 5th I underwent the final surgery on my shoulder (hopefully forever) to plate my Acromion Fracture which had gapped and was not healing. This was an unprecedented surgery for my orthopedic surgeon who has a niche in that field specializing in scapula injuries. He stated that the type of plating and procedure during this surgery for the Acromion Reconstruction nonunion fracture he had not done before, and that this repair was in the top 1-2% of complexities despite having an International referral practice for such injuries.
So I want to take the time to thank the folks involved in my care and surgery while in MN this time around. I tried to take diligent notes. If I missed someone, it was not intentional and I appreciate you just as much.
It all begins with how you are welcomed. When you walk into Regions there is ALWAYS someone there to welcome you and ask if they can help. It makes you feel like they are actually glad you are there…..it’s a great feeling when you are full of anxiety about your visit. It kind of preps you to just go with the flow…so to speak.
To Lonnie and her coworker (nurse that brought me back to preop from waiting room); Aneshtesiologist Dr. Mike Scmid and his nurse Anesthetist Marlene; Pre-op nurses Beckie, and Jackie…..and let’s not forget Lynette F who FINALLY got the IV started successfully; Amelia (who cleaned the surgery site); the Orthopedic Fellow (or Nurse don’t remember) Kyle you guys are all amazing and helped me relax before taking that final plunge to the Operating Room.
To my Trauma team in the Operating Room, including Dr. Peter Cole, THANK YOU for making me better and keeping me alive. I know I am a difficult and complex case. You never gave up on me or dismissed me, or made me feel embarrassed about anything. You are amazing and that is not even a strong enough word to describe your abilities and how much I am truly appreciative.
On the floor the first Nurse I had was named Mike. He had dark beautiful hair and a gentle spirit. He was very attentive along with his PCA Sandra “Sandy” and Bretta the respiratory therapist. I also want to thank Aron for my first meal after surviving surgery. You are a gem. I want to thank Annie for the Aromatherapy and appreciate her professionalism when I did not want her as my nurse due to my January experience with her. I didn’t immediately remember her name…but did her face and voice. Upon reviewing my notes I realized why she was familiar. I want to thank the Charge Nurse of the floor who was a patient listener and got me another Nurse who was awesome to deal with; I want to thank Katie from the lab; and Chian from transport (super nice person who has a relatively thankless job); I also want to thank Amanda, Tim, and Chris from Xray; Dr. Spilseth the Intern who checked in on me in my room; Thank you to Rachel my nurse and her PCA Uniqua; Jennifer from admitting who had the questions about insurance; Kjirsten the Social worker; Brent and Vic from OT and Meghan and Jenny from PT; a thank you to Kidist as well.
I had many wonderful nurses. The list of names was hard to keep track of….I do want to also thank Diana as well along with her PCA Logann (who ran ice packs for me and I am sure was tired of coming in my room); Logann, Dianna, and Patty who replaced Dianna on her shift. I appreciated the rounding from Dr. Hole. I also want to thank Leah and her nurse trainee Sarah and Logann again (yep got me again !); Scott from RT – thank you for checking on my pulse ox and CPAP; Tim and Jessica who did my CT Scan, and Aric from transport…vroom vroom; thank you to my Nurses Netti who took my vitals and said my nurse and pca (Shelly and Lisa) left (without giving a bedside report); thank you to Ketih and Karen; Lynn Charge Nurse and Night Charge Nurse Melissa;
Thank you also to Shelly my nurse and Lisa her PCA (who kept getting Shelly and later Shelly would say that Lisa never got her once and was apologetic) who were late getting me my post op pain meds by over an hour and taught me how much resilience I really have in this tired body.
Thank you to my nurse Melissa and PCA Jonase (spelling might be wrong on this one)…Thank you to Mai, Kaitlyn Schoeck 2nd year Resident and Jocelyn who worked tirelessly to get together all my take home paperwork; Thank you to Marcus Mittelsteadt 2nd year Resident, and the unforgettable Germaine from transport (what a selfless and patient soul) to medical records, and then to the Hotel Bus waiting for us upon departure from Regions after all was said and done.
A special thank you also to Tina Most and the CARE Team as well.
Dr. Cole, thank you for visiting me in my hospital room on Mother’s Day (and a Sunday no less and your weekend off). It meant more than you know. You sat down and explained everything. You rock! You are an Orthopedic Genius. Blessings Abound for you and yours I am sure.
Source: Cinco De Mayo 2016 : Caren Robinson
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
https://hopetbi.com/reviews-and-testimonials/
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
Never Be Ashamed of A Scar.
It Simply Means You Were Stronger Than Whatever Tried To Hurt You…..
Well. Do we have a LOT to catch up on. No I haven’t dropped off the face of the Earth somewhere. Though some days I do feel quite invisible…but that is another post entirely. Trying to keep things real and authentic here and in my mind I have written each update a million times and nothing I felt I could say here matched what was in my head. So tonight, I was just like….well…to heck with it – just be out there with it.
We miraculously by the skin of out teeth made it to MN. We still have not been properly or fully reimbursed for our January, February, or March trip. This has been financially debilitating to us, however, that is not what I want this blog to be focused on.
What I do want to keep the focus on – is the progress and new medical developments that I have encountered, am learning about, and am hoping may help one of you out there in some way. Perhaps someone you even know or have known or will know at some point and time.
So I admittedly have been depressed. On February 5, 2016 I had a PT appt at home. I then had a PCP appt after that. Well, my husband was helping me get dressed, like he has done so many times before. I laid my arm on his arm so he could help get my shirt on me and we heard the loudest POP or CRACK I have heard from a body part. It instantly shot pain up the side of my neck and to my ear. Then strings of pain across my R chest and into my back some. It was dreadful. I couldn’t put my arm down and the pain was IMMENSE. At my PCP’s office she checked me out and reasoned with me that since it “felt” palpably okay that it was most likely recovery pain. I told her it didn’t feel right. I had even called MN that same day on the way to her office to leave a message for Dr. Cole (my orthopedic surgeon). It was on a Friday and since we were going to be in MN on that next week my PCP opted not to xray it.
Well we went…and bottom line is that POP was a BONE being FRACTURED…..a horrible sound I might add. I had apparently fractured my Acromion process (top of my shoulder). Now based on what Dr. Cole explained this was rare (from what we read with our online research – only like 7%- (of course this is rare I thought). He had an xray and CT done. I will say that I have come to realize that xrays have not been incredibly diagnostic for me all along. For some they are better and some they aren’t – me well not so much.
So what did that mean. Well it was aligned for now and I had to do absolutely nothing with it until my next appointment in March to hopefully give it time to heal. Start the protocol all over as if I had just gotten out of surgery. I will say the pain was horrible….but different than shattered pain. I would also say that I am being very well acquainted with a multitude of pain experiences and each have their own level of challenges and differences. How I moved before the scapula surgery that would give me some relief here and there did NOT work for this fracture. I was petrified for it to get separated. If it did get misaligned that would mean potential surgery…This time on the Acromion. We were super super cautious and eventually the neck pain, chest pain and such receeded back into the center of the top of my shoulder to remind me just how broken it was OUCH. But hey… progress is progress. Oh and PT and OT got put on hold. NO Chance of geting that misaligned.
It was a LONNNNNNNNG several weeks. We saw Dr. Cole again on March 16th and this is where we learned That gosh darn fracture hadn’t healed yet and was separated a bit…not by much and he debated just going in to get it repaired and plated while I was there, however it did show bone growth, even though still quite painful and limiting. My head of course was swimming with information and questions that I didin’t seem to be able to get out the way I wanted – so I just listened – not really getting it yet. He decided to cancel the April appointment and then set an appointment for May 2016 to give the body time to do what it appeared to be doing ever so slowly – trying to heal itself. That meant however, no weight bearing at all with my right arm though I could begin again with PT conservatively.
So in May we find out whether I stay for a bit to plate this bad boy and fix it for good, or whether nature has taken its time, but actually healed it properly. That appointment feels like its lightyears away.
There is actually some awesomely good news in all of this though. There is a LOT less pain in my scapula. Like it is miraculous how much he helped me with those January surgeries so I have utter faith in this man – even if I do have to have another surgery I know….like truly know he will make it better.
I am still quite limited but that will just take time and lots of therapy to get my strength back up. We don’t know how much of the nerve damage will remain, continue to affect things, and all that stuff. Time will tell. I will say that it just flooded me like
REALLY MORE BROKEN STUFF!!!! It was a lot to absorb and focus on in a positive way. After a while, even though I know things were feeling different in some ways and better…..they were worse in other ways and status quo in yet other ways. Also fighting with Insurance to get basic quality of life and such should not be a constant fight and battle. This just adds to the stress and I truly believe slows the healing process because now you are always focused on that next ball getting dropped by them….it’s distracting, annoying, and is something that needs reformed for sure. That’s my soapbox on that though.
So here we go. Working hard to stay afloat. Not just financially but in the dynamics of our relationships with each other in the house. The trips are hard on my body and my brain. I think I am going to end up with the back pain for life. The headaches are crazy consistently unrelenting and so mch a part of me now that I don’t remember when I last never had one.
I feel so flooded and overwhelmed after I get home fro travelling that I literally crash out and sleep like I haven’t had sleep in days. Going each way usually takes me a few days to play catch up with my already seemingly dulled self. There is so MUCH stimulation that I was never aware that I was aware of before. Travelling def makes a difference. I have totally decided that travelling by train is much less intense than by Plane. Still tons of people and still tons of noise and activity, but we get our own room which helps quite a bit with trying to get a grip…..and it is way more economical.
We keep moving forward….making impossible choices….going with the flow Time and time again. The future uncertain, but glad that I am still here to have a future to be uncertain about…..
So sorry for the delayed update – more posts to come…..just been battling exhaustion, pain, fatigue, and a good dose of BLAH!
Article – Time and Time Again by Caren Robinson
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
https://hopetbi.com/reviews-and-testimonials/
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
This is how amazing my Orthopedic Surgeon from MN and his team’s are. He is the one who jus completed two surgeries on my scapula and reconstructed it with a bone graft.
They truly care about their patients; and I am a growing strong advocate of their work and care as a whole both State Side and Away….
This is the charity Dr. Cole and his wife started:

Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
https://hopetbi.com/reviews-and-testimonials/
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
Hello. In MN January 11-24, 2016. It has taken me this long to get my energy up enough to type an update…..
I apologize that it has taken me so long to come to give all of you an update since my surgeries. I also must apologize for any horrible writing or spelling…I am still on the mend. First I want to sayis HALLELUJAH i AM ALIVE!!!
This has been quite the experience and it will continue to be. More posts will follow this one, however for this one I want to address some special folks. I tried to keep track the best I could with my notes. I truly apologize if I miss your name.
Specifically to My Primary Care Physician and her office staff; my Counselor, Mercy Medical Angels (especially Steve Craven), Barry and Caryn Mehler (dear Friends), Mary Herndon-Williams (sister from another mother), Priscilla Benavides and her husband (an old soul friend), Karleen Robinson (my mother-in-law), Carly Kissinger ( a teacher), and Samantha Rogers (Trauma Survivor), and the Rabbi from Ahavas Israel in Grand Rapids, MI; and Unity Center for Spiritual Growth in Ada, MI; United Airlines and its many wonderful staff and crew, Gerald R Ford Airport out of Grand Rapids, MI to Chicago O’Hare (in nowhere else but Chicago, IL) to Minneapolis St. Paul. Minnesota and those of you who pushed my wheelchair – THANK YOU FOR GETTING ME THERE SAFELY. Without your help and support my arrival would not have been possible. To the gentlemen in 1st class who gave up your seat for me because I looked so uncomfortable in coach from Chicago to St. Paul – mere words are not enough to give you my deepest gratitude. You are a gem.
When we arrived. An enormous thank you to Yellow Cab, Embassy Suites, UBER, SuperShuttle, the hospital shuttles, delivery folks, and the beautiful people of St. Paul who made a very scary and lonely time not so scary and not so painful for my husband and myself. Thank you Unity in the Heart Church in St Paul, MN.
THE GOOD STUFF – MEDICALLY LAIDEN
To my EMG team and Dr. Olson at Regions hospital, the Radiology Department, the lab, Medical Records and the Welcome staff – thank you for being quick and efficient and accommodating.
Veronica the bone specialist and Dr. Pegrow from Infectious Diseases – you guys are amazing and taught us a lot. Thank you Charge Nurses and Patient Relations and for the Alternative Medicine that compliments the Allopathic side of things. This made a world of difference for me and helped manage my fear, anxiety, and pain..
For my miraculous Dream Team with Health Partners, Regions Hospital, my Orthopaedic surgeon Dr. Peter Cole (our dedicated man of God and Science) who made all this possible for so many like me AND ME, Tricia Corbo, Jenny, Tina Most, his two fellows Dr. Hesse and Dr. Diskin, the Anesthetist and the Nurse Anesthetist and all the office and team members whose names I didn’t write down, don’t remember or I don’t know in the office, this process and in the Operating Room – thank you for helping fix me and for keeping me alive to face another day. Your hands are truly the extension of the hands of God himself and I value and am grateful for each and every one of you.
For the floor staff thank you to Dr. Campbell (you were a sheer delight), Dr Brenner (miss that beautiful long hair 🙂 ty for your compassion), Dr. Mehta (kind eyes and soft smile); Brigid PT and Lena OT and lets not forget the folks that make the Doctor’s work look flawless and managed my pain and care in a more extended way – my NURSES Alena, Stella, Annabelle, Megan, Jessie, Abbey, Kasie, Niki Z (or2),Rachel, Rin, Rose, Leann, Brian and Kristy – Annie I forgive you for missing my meds for the whole night….it was a good lesson for me not to miss my scheduled doses – even good comes from mistakes…..forgive yourself and move on.
Also my Nursing Assistants they call PCA’s in MN: Fey, Hanna, Sandi Nettle, Laura, Dominique, Lisa, Mollie, Crystal, Lindsay, Nalee and any others I may have missed while sleeping or being to groggy to write. You were my hands when I couldn’t and my extended family while away.
To my husband Rick Robinson and soulmate and best friend – thank you for braving the trip, this uncertain future, and for sacrificing so much of yourself and your time, and your sleep for me. I know it takes so much from you and you deserve more than I could ever begin to repay you. I love you and value every moment with you. Thank you for believing in me and not doubting me all along through this whole shabang.
To my family who waited for me at home, for my darling children, for those who lovingly cared for my children while Rick and I were gone…..Thank you and I appreciate the support , love, and prayers.
I am home dear ones I am home! I am so eternally grateful and not last or least, but thank you Heavenly Father for granting me purpose in this world and allowing me to carry on another day to tell this story and continue to recover.
Follow up appointments in MN with Dr. Cole on February 10, 2016, then at 6 week mark – then 3 months, 6 months, 9, months, and 12 months. We are grateful for these opportunities to watch miracles abound and grow.
The two surgeries are reconstructive procedures for the nonunion scapula fractures (shattered unhealed scapula I have). The surgeon has done many of these types of surgeries involving complications of scapular fractures, nonunions, malunions, delayed treatments, etc.
The current proposed plan is a 2 stage surgery. The first will involve cleaning out the nonunion site and obtaining bone and soft tissue cultures to be sent for bacterial analysis. He will then place antibiotic beads and then after 5 days in the hospital he will then do the grafting procedure from the iliac crest (pelvis). Waiting that duratino insures a steril environment for him to perform the bone grafting procedure and place the foreign body implants. The second surgery also includes correction of the instability and the malalignment of my shoulder blade. Stainless steel plates and screws will be used in addition to the bone grafting.
The track record for these surgeries is well documented in the literature, of clinical research coming from his practice. He feels the outcome is estimated to be between good and excellent regarding this injury.
Afterwards there will be about 3 months or so of Physical and Occupational Therapy.
I am looking forward to having use back of my right arm with full range of motion. I am looking forward to managing this ongoing debilitating pain and miserable aura.
Godspeed to the hands of the surgeon and his whole team that are making this possible. Godspeed to my husband who will be by my side throughout this ordeal. We have to travel out of the State as Michigan – as Michigan State does not have any surgeons who do this specialized procedure. The kids are already getting anxious and prepared. Rick and I are stilll trying to wrap up loose ends before we have to go.
Intense stuff, however opportunities full of HOPE. Help One Person Excel – To Be Independent.
Thank you all for reading this, being a support and following our process. Please feel free to leave comments below, or share this post on your social media.
Blessings Always.
Caren Robinson – Polytrauma Survivor

(Note: The picture on this post is the actual hospital where I will be having my surgery. They implement several safety steps during the surgery process – this is very encouraging to me)
Happy Anniversary to my ReBirthday today.
Today, this date 2 years ago I was involved in a catastrophic car wreck that changed the life of myself and my family and I was given a special gift of life and additional time with my family.
I am beyond blessed to have been given these extra months with my husband, my kids,and my family.
The Journey Continues…I am A Survivor!!!
Survivors, Caregivers, Providers –
If you want your story shared/published on this site, let me know. I am a Survivor trying to bring inspiration and awareness about TBI to others.

Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
Reviews and Testimonials
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
I just learned within the last week that there was news footage about the wreck I was in with my son. The wreck that changed the course of many more lives than just the 3 people (myself, my son, and the other driver) directly involved in the wreck. It would change the life of everyone that was involved that day. Whether a good Samaritan, police officer, or EMS/Fire.
I am still in the throws of processing this new information myself. New to me anyway. Anything that may have been told to me before about it, I have no existing memories of.
So it has been 20 months and 9 days since the wreck as of this writing. I do not know why I didn’t know about the news coverage until recently. Once I found out, I tried looking all over for this information. I am glad I found what I did. I am learning more every day. This has been essential to my recovery.
I found out that it had been indeed published on Channel 3, Channel 17 (FOX), and Wood TV 8. I also found out in the online search that a gentleman had also taken video footage of the scene towards the end of the rescues and posted this to youtube.
The discovery of the youtube video was a long awaited blessing. The information provided was crucial and substantial to me and my family. It was snowing, the roads appeared icy, and as we would have confirmed for us it was very cold and windy as well. Apparently I was already being taken to the hospital when he started filming. You see a couple of spots on the video that show his windshield wipers going. You also hear dispatch communication at 1m:39sec that speaks of the extrication being completed and now they are going to clean up. Dispatch says it is 12:42 (when extrication of other driver was completed).
Listed below is what the videographer wrote on his youtube synopsis of the video he posted:
Wyoming fire dept on scene of a head-on-crash on Gezon parkway near Byron center ave.
There were two patients 1 was ejected and the other was trapped in the car. a Chevy Silverado truck collided with a chevy cavalier both victims were priority 1 taken to the hospital. Police are investigating.
Units on scene were: engine 77, medic 87, AMR, 3 Wyoming police cars, and reserve engine 79 all Fire units were from Wyoming station 4. Thanks for watching please comment like or subscribe and be safe in the weather ahead. P.I with entrapment and ejection on Gezon ( video here)
[the van was actually a Chevrolet Venture, however, yes – the car was a Chevrolet Cavelier]
and the journey continues…..I will share more as I know it and am able
Today I have my first appointment with a Pain Clinic. I am not even sure what to expect. However, will let you know how it goes.
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
Reviews and Testimonials
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.
This Website is a gift of love. To myself, to my husband, to my mom, my children, and all those that have been touched by trauma in any form. To those who have cared for me or tended to me in any way, I continue to learn something from each person I come into contact with. Even those I may not readily remember.
When I came home from the hospital….my body was home, but not all of me….not really. I am getting to learn the “new” me, while remembering the me I used to be. Welcome to a glimpse into the world of having a TBI (Traumatic Brain Injury) among other things. The steps in this tumultuous journey I will share with you in these pages, as time goes on. Thank you for reading this blog. Welcome. Come on in, stay a while.
Thank you for visiting the HOPE TBI Website.
Please take the time to make a comment, share your thoughts, and tell us what impacted you the most and what brought you here:
https://hopetbi.com/reviews-and-testimonials/
Your input is important to the development and growth of this website, and we like to know what is going on out there in your thoughts.
Thank you for visiting us! We look forward to hearing from you.